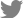|
 |
| jbm > Volume 30(3); 2023 > Article |
|
Abstract
Dental pulp stem cells (DPSCs) have garnered significant interest in dental research for their unique characteristics and potential in tooth development and regeneration. While there were many studies to define their stem cell-like characteristics and osteogenic differentiation functions that are considered ideal candidates for regenerating damaged dental pulp tissue, how endogenous DPSCs respond to dental pulp injury and supply new dentin-forming cells has not been extensively investigated in vivo. Here, we review the recent progress in identity, function, and regulation of endogenous DPSCs and their clinical potential for pulp injury and regeneration. In addition, we discuss current advances in new mouse models, imaging techniques, and its practical uses and limitations in the analysis of DPSCs in pulp injury and regeneration in vivo.
Dental pulp stem cells (DPSCs), a subpopulation of mesenchymal cells, have emerged as a promising therapeutic tool in dental tissue repair and regeneration. Specifically, postnatal DPSCs play an essential role in supplying differentiating odontoblasts that line the pulp chamber and are responsible for the formation of dentin; the hard and mineralized tissue that makes up the bulk of the tooth.[1] Dentin provides structural support and protection not just to the dental pulp, which houses DPSCs but to the overall tooth as well.
The traditional approaches to study DPSCs mainly used in vitro experiments where DPSCs are isolated from dental pulp tissue and cultured under controlled laboratory conditions. These studies focused on characterizing morphology, growth rate, and differentiation potentials of DPSCs. These in vitro studies also investigated DPSC regenerative capabilities by looking into their proliferation, migration, and secreted regeneration-associated factors.[2-4] However, despite providing valuable insights, these traditional in vitro approaches have many limitations, including the lack of in vivo complexity, limited physiological relevance, and simplified injury models, resulting in non-translatable findings to clinical applications. Compared to in vitro approaches, in vivo studies provide stronger evidence for the clinical translatability of stem cell-based therapies. In vivo studies also allow us to characterize DPSCs in their natural microenvironment, interactions with other cells and extracellular matrix, and in response to endogenous signaling molecules. Furthermore, in vivo DPSC studies can provide more consistent and reproducible results with safety and efficacy evaluations in preclinical models, which will undergo more in-depth clinical trials.
Despite these advantages of in vivo studies, how DPSCs respond to dental pulp injury has not been extensively investigated in vivo. This is mainly due to the lack of animal models and standardized methods to generate and quantify dental injuries in vivo.[5] Therefore, the development of in vivo pulp injury models and the study of DPSCs under physiologically relevant models are essential for a more comprehensive understanding of DPSCs’ regenerative capabilities. Among the different animal models that have been used, genetic mouse models present many advantages such as availability, cost-efficiency, ease of handling, reproducibility, and the presence of various transgenic or mutant models.[6] Understanding the in vivo regulatory mechanisms of DPSCs will contribute to the development of novel therapies for dental tissue repair and regeneration, thereby revolutionizing the field of dentistry and oral healthcare.
In this review, we will discuss the current knowledge about the role and regulation of DPSCs in tooth development and regeneration, the current in vivo mouse models used for investigating pulp injury regeneration, and the different categories and methods for pulp injury creation. We will also discuss the responses of DPSCs to pulp injury in vivo, its applications, and future directions.
Mouse jawbones and teeth are crucial components of the oral cavity. Upper jawbone (maxilla) and lower jawbone (mandible) contain sockets (alveoli) that hold teeth firmly in place. Mice have 2 upper and 2 lower incisors located in the frontal midline of each jaw. Mouse incisors are the first teeth that emerge from the gumline and are easily visible when the mouth is open (Fig. 1). On both sides of mouse incisors, 3 molars are arranged in a row from front to back deep in the oral cavity, for a total of 6 molars per jawbone. Small oral cavities of mice and large frontal incisors are a major challenge to access to the rest of the cavity and molar teeth.
Each tooth is divided into 2 sections, the crown and the root. In molars, the crown is the visible portion of teeth above the jawbone, while the root is anchored into the jawbone. The root of teeth extends deep into the jawbone and is closely associated with important nerves and blood vessels, which must be carefully protected during surgical procedures. In incisors, the crown analog is the lower half, and the root is the upper half of its longitudinal section (Fig. 1). [7] The crown is covered by enamel, which is the hardest body substance. This protects the crown from injury despite the constant grinding or chewing and prevents injury or infection from penetrating the underlying components of teeth. On the other hand, the root surface is covered by a specialized tissue called the cementum. The root of each molar is anchored in the jawbone by periodontal ligaments (PDLs), which help to cushion teeth and maintain tooth position in the socket. Immediately inside the enamel and cementum, the dentin can be found surrounding the dental pulp.[8] The dental pulp is a soft connective tissue found in the center of incisors and molars. During the development, DPSCs contribute to dental pulp formation. In turn, DPSCs in dental pulp can differentiate into various cell types, such as odontoblasts and pulp fibroblasts, making dental pulp an important structure for maintaining tooth vitality and responding to injuries and infections.
While mouse incisors and molars share some similarities in their overall structure and function, the key difference is in their postnatal growth patterns. Incisors grow continuously throughout the animal’s life, with new tooth formation at the base of incisors and old tissue being worn away at the tip of incisors. In contrast, molars only grow one time and develop during specific stages of the animal’s life. Differences in the genes and signaling pathways that control the growth and differentiation of tooth stem cells may lead to the different characteristics observed between incisors and molars. However, adult human teeth are more like mice molars than incisors as they do not spontaneously grow and regenerate.
The tooth harbors various stem/progenitor cells. Aside from DPSCs, stem cells from human exfoliated deciduous teeth (SHEDs), PDL stem cells, dental follicle stem cells, stem cells from apical papilla, and gingival mesenchymal stem cells were identified.[9] Among all of them, DPSCs and SHEDs are found to be the major sources of odontoblast progenitors during dentin injury repair,[10] while DPSCs are the major player in the regeneration and revascularization of the pulp tissue.[11] DPSCs also offer distinct advantages, including accessibility and abundance compared to other stem cells. They can be obtained from extracted or naturally shed deciduous teeth. The self-renewal capability of DPSCs enables them to divide and generate more stem cells, providing a sustainable cell population for regenerative therapies and therapeutic interventions in dentistry.[12]
DPSCs play a crucial role in tooth development and regeneration. DPSCs are derived from the dental papilla, a cluster of cells located in the pulp at the center of the tooth bud during the developmental stages of the tooth. Gronthos and colleagues [2] first isolated DPSCs from postnatal human third molar. These DPSCs are similar to the bone-marrow-derived mesenchymal stem cells (BMSCs) due to their clonogenicity and proliferative properties. Further, they possess BMSC features, including the ability to differentiate into various cell types and the ability to modulate immune responses and promote angiogenesis. However, unlike BMSCs, these DPSCs have a unique function to form a dentin/pulp structure complex after transplantation in the dorsal surface of immunocompromised mice.[13] During tooth development, DPSCs undergo a process called differentiation, where they specialize in different cell types that contribute to specific components of the tooth structure.
DPSCs originated from multipotent cranial neural crest cells (CNCCs) responsible for the development of the craniofacial complex in vertebrates.[14] CNCCs have a lineage bias towards mesenchymal cell fate in tooth development. During the embryonic stage of mouse tooth development, dental epithelium elongates and invaginates into the underlying CNCC-derived dental mesenchyme associated with mesenchymal condensation. The condensed mesenchyme becomes the dental papilla and the epithelium starts to surround it. The DPSCs in the dental papilla then give rise to the dental pulp and odontoblasts.[7,15,16] During this process, DPSCs express multi-lineage markers, such as endothelium (i.e., Vcam1, CD146), bone (i.e., alkaline phosphatase [Alp], type 1 collagen [Col1]), fibroblast (i.e., Col3), and smooth muscle (i.e., α-smooth muscle actin [Sma])-associated markers.[2] DPSCs also express BMSC markers, such as CD73, CD90, CD105, and Stro1.[17-19] The co-expression of α-Sma, CD146, and 3G5 in DPSCs suggests their perivascular location in dental pulp. Several in vitro culture studies have shown that DPSCs have odontogenic differentiation potentials with the expression of common odontoblast markers; Alp, Col1, osteopontin, osteocalcin, dentin matrix acid phosphoprotein 1 (Dmp1), matrix extracellular phosphoglycoprotein, and dentin sialophosphoprotein (Dspp).[20,21] Other studies revealed odontogenic-inducing factors and cytokines for DPSCs such as insulin-like growth factor (IGF), fibroblast growth factor (FGF), transforming growth factor-β (TGF-β), vascular endothelial growth factor (VEGF), platelet-derived growth factor, epidermal growth factor, dental epithelium-derived protein copine gene 7, endothelial cell-secreted endothelin 1, and bone morphogenic proteins (BMP).[22-25]
DPSCs are heterogeneous cell populations that continue to contribute to dentinogenesis postnatally. Recent single-cell (sc)RNA analysis of mouse incisors and mouse and human molars showed different clusters of DPSC subpopulations expressing different markers and transcriptomic profile.[26] In the mouse incisors, pulp progenitor populations encompass apical pulp and distal pulp cells that are distinct from mature odontoblasts. The apical pulp progenitor cluster has a diverse pool of stem and stromal cells expressing Thy1 and Gli1 genes which are linked to self-renewal properties, and cells expressing the proliferative gene marker Mki67+ with Fgf3 and Foxd1.[27,28] Recently, Foxd1 has been identified as a new marker for DPSC subpopulation located in the apical papilla near the cervical loops. In contrast, the distal pulp progenitor cluster contains progressively differentiating cells finally expressing Igfbp5 and Syt6.[26]
In the mouse molars, pulp progenitor cells are divided into the coronal (Enpp6+/Fabp7+), middle (Nnat+/Rab3b+) and apical (Aox3+/Tac1+/Fgf3+) subtypes.[16] DPSCs, specifically the apical papilla subtype, continue to form dental papilla and odontoblast postnatally. Using Fgfr3CreERT2;tdT mice, Jing and colleagues [16] were able to track Fgf3+ cells in the dental pulp and odontoblasts of P3.5 mouse molar. Fgf3 was found to specifically label the apical dental papilla and stimulate dental mesenchymal stem cell (MSC) proliferation which is important for stem cell niche maintenance.[16,29] On the other hand, coronal dental pulp cells can form odontoblasts specifically in post-injury repair, emphasizing the unique regulation and functionality of DPSC subpopulations. Similarly, human molar pulp cells have multiple cell clusters representing MSCs, odontoblasts, endothelial cells, Schwann cells, immune cells, epithelial-like cells and erythrocytes.[30,31] Several studies have also shown the osteogenic potentials of DPSCs, implicating DPSCs as a promising candidate for stem cell therapy in bone diseases or defects specifically in the craniomaxillofacial area.[32]
DPSCs are reported to contribute to root development and the formation of supporting structures of tooth.[33] DPSCs differentiate into cementoblasts, which produce cementum. Cementum is a specialized tissue that covers the root surface of the tooth and helps anchor it to the surrounding jawbone. A subset of early pulp stem cells also contributes to forming the PDL, which consists of collagen fibers that connect the tooth root to the surrounding bone and enable the tooth to withstand chewing forces. The underlying mechanisms of odontoblast, cementoblast, and PDL differentiation, as well as reparative dentinogenesis remain elusive. In addition, the interaction between DPSCs and other pulp cells and the regulatory molecules from their microenvironment remains to be further investigated in the natural in vivo setting.
The regulatory mechanisms of DPSCs are multifaceted and controlled by various factors and signaling pathways. Notch, Wnt, BMP, and Hedgehog pathways are known to play a pivotal role in regulating DPSCs. These pathways govern their self-renewal, proliferation, and differentiation processes. In addition, transcription factors such as Oct-4, Nanog, Sox2, and Klf4 are reported to maintain the stemness of DPSCs by controlling gene expression patterns to balance DPSC self-renewal and differentiation.[34-36] Epigenetic modifications, including DNA methylation and histone modifications, also contribute to the fate and behavior regulation of DPSCs.[36,37] Further, DPSC niche factors, the local microenvironment surrounding DPSCs, play a pivotal role in their regulation. Their niche factors include the extracellular matrix, cell-cell interactions, and soluble cytokines secreted from neighboring cells.
Different tooth may have different environments and growth regulation. Further, at the different stages of tooth development, different combinations of growth factors and cytokines can modulate DPSC proliferation, differentiation, and their responses to environmental changes. For example, while TGF-β, FGF, and VEGF are well-known growth factors for DPSCs, the apical incisor DPSCs selectively express Sfrp2, Lef1, Fzd1, Sfrp1, Rspo1, Trabd2b, Gli1, and Wif1 genes which are related to tooth regeneration and production of a hard matrix during physical injury.[26] These factors can stimulate or inhibit apical DPSC proliferation and influence their odontoblast differentiation potentials. Further understanding of specific regulatory networks of DPSCs and manipulation of these mechanisms will harness the full regenerative potential of DPSCs for various applications in regenerative medicine, tissue engineering, and dental therapies.
Earlier studies to investigate the regeneration potentials of DPSCs were based on in vitro and ex vivo experimental approaches.[38] Later, in vivo approaches were then developed to verify results from existing literatures and to generate more physiological and reproducible data.[2,39] These in vivo models can be classified into 2 categories: ectopic and orthotopic. In ectopic models, DPSCs with or without bioactive scaffolds and factors are implanted in the dorsal area of the immunocompromised animals, commonly rodents.[40] On the other hand, in orthotopic models, DPSCs are transplanted into dentinal injury or dentin and pulp injury of tooth. Commonly used technique are the pulp capping method in which bioactive materials mixed with cells are directly implanted into minimally exposed healthy dental pulp.[39] Recently, a modified pulp capping model for dental injury has also been introduced. In this approach, a bioactive cement such as mineral trioxide aggregate (MTA) is applied to the injured dentin/pulp and sealed with a glass ionomer or composite resin without any DPSCs.[39,41,42] This approach may enable researchers to investigate new pulp tissue formation from endogenous cells.[39]
Recently, transgenic mouse models have been increasingly used in the studies of endogenous dental pulp development and regeneration. The deletion of TGF-β receptor 2 (TGF-βr2) and Klf4 in Wnt1-Cre mice showed decreased odontoblast maturation, dentin formation, and decreased Col1a1, Dspp, Dmp1, and Osx expression.[36,43,44] Further, high Gli1 expression was detected in the apical papilla subpopulation of the DPSCs.[45] BMP receptor 1 (Bmpr1) knock-out in Gli1-CreER mice impaired root development and absent Dspp expression in the apical molar. Gli1CreER;Bmpr1αfl/fl; tdTomato fluorescence reporter mice showed reduced apical migration of the cells. In addition, lineage tracing of Gli1+ DPSCs identified an NG2+ perivascular subset in the incisor and as a transient root progenitor in the molar.[28] Deletion of the transcription factor, paired-related homeobox gene 1 (Prrx1), also affected molar morphogenesis producing ectopic epithelial projections, cervical loop hypoplasia, and cuspal patterning defects.[46] This suggests that Prrx1+ cells are important in tooth development and represent a dental stem/progenitor population, similar to Prrx1+ stem cells present in the long bone periosteum and calvarial suture.[47-49] Lastly, αSMA-green fluorescent protein (GFP) transgenic mice showed the presence of GFP+ cells in the molar and incisor dental pulp from P7 to 6 weeks of age. These cells express Sca1 (a MSC marker) and are involved in odontogenesis during growth and development.[42]
The use of transgenic mouse models in combination with recent in vivo dental pulp injury models is a promising approach to characterize DPSCs in their natural environment and to unravel the underlying mechanisms of their regenerative responses.[43] However, postnatal tooth pulp is composed of highly heterogenous cells. Therefore, there is an unmet need to define specific genes and markers for endogenous DPSCs. Mouse models for adult skeletal stem cells (i.e., Mx1-Cre) [50] will be useful resources to investigate adult DPSCs during dental injury.
Tooth injury can be classified based on the location and degree of tissue damage. The endodontic Ellis system of dental trauma can be used as a guide to dentin/pulp injury.[51] Ellis Class I involves a complete fracture of the enamel without dentin exposure. Ellis Class II is the injury with dentin exposure making pulp vulnerable to contamination even though it is not directly injured. Ellis Class III are full-thickness fractures with pulp exposure and associated bleeding. Byers and Närhi [52] introduced another classification of dentin/pulp injury for animals which is more complex than the Ellis system (Fig. 2). Type I or mild/transient injury creates a mild superficial dentin injury stimulating reactive dentinogenesis. In this mild to moderate type, odontoblasts adjacent to the site of injury produce reactionary dentin, a type of dentin that is formed rapidly in response to injury. Type II or intermediate injury involves deeper dentin injury with partial pulp loss stimulating reparative or tertiary dentin formation. Many odontoblasts are affected in this more severe type making them unable to produce sufficient dentin to protect the pulp tissue. In these cases, newly differentiated odontoblast-like cells derived from DPSCs can replace the lost or damaged odontoblasts and produce reparative dentin to fill the pulp chamber, promoting tissue repair and regeneration (Fig. 3). Lastly, Type III or irreversible pulpitis involves large pulp exposure or coronal pulp destruction which highly induces advancing necrosis and systemic defense reaction. To investigate response of DPSCs in dentin/pulp injury, type I or type II injury is recommended.
Several factors affect the outcome of injury creation, such as the site of the injury, variation in animal oral cavity and tooth, the actual method for injury creation, and the skill of the surgeon. The injury tool, speed of injury creation, control of heat, and damage to adjacent tissues are some of the factors that can affect the injury and subsequent regeneration and thus injury methods should be standardized.
During a mouse oral surgery, a stable and secure surgical bed is essential to minimize movement and provide appropriate angles for visualizing the oral cavity. Traditional instruments such as tweezers and needle holders are unsuitable for securing the intraoral visual field for prolonged periods, as they require both hands of the operator. A custom-made dental board, which typically consists of a small, flat platform with a slot or groove to accommodate the animal’s head, as well as clamps or straps to hold the head securely in place, is a popular option for a mouse oral surgery bed.
Early designs of mouse surgery beds mainly focused on securing a working field of view, but recent developments have led to more advanced and customized designs for enhanced precision and efficiency during mouse oral surgeries. Recent advancements in 3-dimensional printing technology have enabled the development of custom-made surgery beds tailored to researchers’ specific needs.[53]
A well-designed surgery bed should not only enable secure positioning but also allow for adjustment of head angle for better visibility and easier access for anesthetics delivery during respiratory anesthesia. Also, dental beds have been successfully utilized in various dental procedures in mice, including tooth extraction, periodontal inflammation surgery, and pulp capping.
In order to access the teeth of a mouse, particularly the molars, the use of a mouth gag or a similar device is necessary. The mouth gag is placed in the mouse’s mouth, with the upper and lower incisors resting on the metal arms of the gag. Adjustments should be made to ensure the comfort of the mouse and to prevent injury to the teeth and surrounding tissues. The tongue should be gently pulled forward to improve the visibility of the teeth. Another option is the use of a mouse-gagging appliance, which is specially designed to secure the field of vision for various surgeries while minimizing interference with tongue movement, rodent size, and mucosal location.[54] To achieve more precise positioning and stabilization during the procedure, the use of a stereotaxic frame is also an option.[55-57] The stereotaxic frame is particularly useful for studies that require precise targeting of specific areas of the mouse’s mouth or teeth, such as studies on dental caries or periodontal disease and leads to improved accuracy and reproducibility of experimental results.
In studies involving tooth pulp injury, various methods have been developed to inflict injury on animal teeth.[58] Due to the complicated anatomical structure of the mouse tooth and its relatively small size compared to other animal models, however, a careful and precise approach is crucial during surgery to create an accurate and appropriate injury. The selection of an appropriate tooth pulp injury method, considering the size, depth, and intended purpose of the injury, is also essential for studying the mechanisms involved in dental pulp injury and regeneration. The current standardized method for inducing tooth injury in mice has been utilized for the past decade. These procedures involve 3 distinct steps: cavity formation, pulp opening, and cavity sealing (Fig. 3). Recently, other injury methods with newly developed methodology, which we initially examined, have been introduced as alternative approaches to current protocols (Fig. 4).
Injury by automatic drill is the most commonly used and reliable method for inducing pulp injury in mouse models. A high-speed handpiece is used to create a cavity on the surface of the tooth.[41,42,59-61] The position forming the cavity can be designed in various ways according to the purpose of the experiment. In the case of molar, it can be the tip of the pulp horn, the occlusal groove, or the lateral plane close to the root. For incisors, maxillary and mandibular crown parts and lateral planes are preferred. A diamond bur is used to drill the cavity, and the exposed dentin is removed using a spoon excavator.
The advantage of this method is that it allows for precise control over the extent of injury and the location of the injury site. The use of a high-speed handpiece and diamond bur ensures that the cavity is created quickly and efficiently, minimizing the risk of heat buildup and pulp and DPSC damages. However, the use of a high-speed handpiece can create vibration and heat, which may damage the surrounding tissues and compromise the accuracy of the injury. In addition, when using a high-speed handpiece, heat generation must be minimized while receiving water with phosphate buffered saline, and at the same time, appropriate water suction must be performed, resulting in spatial limitations and the possibility of suffocation of the animal model. As an alternative to a highspeed handpiece to generate cavity, a poking method using a low-speed handpiece or fine needles can be considered.[62-65]
In the case of a cavity extending up to the dentin, even if the pulp is not exposed to the outside, DPSCs and pulp cells can have injury response due to the indirect pressure of the dentinal tubule or mechanical force present in the dentin. However, when pulp opening occurs, immediate inflammation and more distinct cell responses are observed.
Pulp opening can be induced during cavity formation, but it is very difficult to make an opening of a certain size. In addition, if the injury caused by an excessively deep cavity or a high-speed bur is severe, it induces DPSC and pulp cell necrosis, making it difficult to obtain the desired experimental results. The most commonly used pulp opening strategy is the method of using an endodontic file in endodontic practice. The endodontic file is thick enough to form a small opening of 0.08 to 0.15 mm. It also has a length of about 30 to 50 mm, so it has high accessibility to the injured area. A sterilized endo explorer can then be used to advance into the opening until the pulp cavity was encountered.[66] The process of pulp opening utilizing an endodontic file necessitates a considerable level of proficiency due to the precise manipulation required to achieve the desired depth and dimensions of the cavity. Additionally, it bears a substantial risk of infection, thus necessitating utmost vigilance and adherence to cautionary measures.
Dentin and pulp tissue exposed to the outside are potentially exposed to saliva, so they need to be sealed due to the risk of infection. There are several options for materials that can seal the cavity, but a small amount of flowable resin for sealing the opening is preferred.[42,67,68] In order to promote the regeneration efficiency of the pulp, MTA cement, which has been widely used for patients recently, is also one of the options as a filling material.[42] Using a new material or molecule in this filling step can be conjugated to compare and confirm the healing capacity in the preclinical stage in the field of dental materials.
Aside from mechanical drilling, there are other possible approaches to see injury response. One technique is air abrasion, where a stream of air combined with abrasive particles is used to remove decay or prepare the tooth surface for restorative materials.[69,70] Laser dentistry is also an option, utilizing precise laser beams to remove or shape tooth structure without anesthesia in some cases.[71,72] Additionally ultrasonic instruments utilize high-frequency vibrations to remove damaged tooth structure or clean root surfaces,[73,74] while microabrasion involves the application of a mild acid and abrasive agent to eliminate superficial enamel defects or discoloration.[75,76]
Recently, a novel methodology has been introduced, which involves the utilization of a hand-operated micro drill bit for the purpose of inducing injury.[64] This marks the first instance where such a technique has been proposed (Fig. 4). The use of a micro drill bit for cavity formation presents several advantages over machine-based methods. Firstly, it allows for the creation of cavities with utmost precision and standardization while minimizing undesirable side effects such as heat generation and spatial limitations. Moreover, during the initial stage of pulp opening, a thin drill bit (range, 0.1-0.2 mm) can be employed continuously, thereby achieving outcomes comparable to those obtained with an endodontic file. Previous investigations employing a fluorescent mouse model have demonstrated the occurrence of injury response in pulp, DPSC, and odontoblast cells. Furthermore, it has been confirmed that this novel approach exhibits a lower failure rate (perforation) and enables consistent cavity formation compared to the existing protocol.
These alternative methods for managing tooth injuries provide less invasive options than the drilling techniques above. However, it is important to note that the specific method chosen depends on the type of study and DPSCs response investigated, as well as the researcher’s expertise and available equipment.
The in vivo response of tooth pulp cells, including DPSCs, to injury is a critical determinant of tissue regeneration and repair. Following injury to the dental pulp, tooth pulp cells undergo a series of cellular and molecular events that ultimately result in the formation of tertiary dentin, which protects the underlying pulp tissue. Recent studies have highlighted the crucial role of DPSCs in tertiary dentin formation.
Angelova Volponi et al. [77], Neves and Sharpe [78] did a series of in vivo dental pulp injury studies using Axin2 as a marker for dental pulp cells. A cavity was drilled in the center of the superior first molar using a carbide bur with high-speed hand piece just enough for the pulp to be visible under the dentin roof. A 27 gauge needle was then used to expose the pulp chamber, filled with MTA, and sealed with glass ionomer. They found that Wnt/β-catenin signaling drives reparative dentinogenesis by using Axin2LacZ/LacZ mouse model. Similarly, they observed enhancement of dentin formation with the treatment of glycogen synthase kinase-3 inhibitor with a collagen filling solution.[59] In a subsequent study, they showed that Axin2+ cells have DPSC proliferative capacity and ability to differentiate into new odontoblast for reparative dentin formation.[41] Supporting the involvement of Wnt/β-catenin signaling, Axin2CreERT2; Wlsfl/fl mice had reduced cell proliferation in response to pulp exposure compared to wild type due to inhibition of autocrine Wnt release. Surprisingly, the inhibition of other known odontoblast-inducers such as TGF-β and BMP2 was found to not affect reactionary dentin formation but resulted in a more disorganized, nontubular dentin.[78] This emphasizes the need for more in vivo injury studies to verify previous data from in vitro and in vivo non-injured models.
Other study with fluorescence reporter mice revealed that αSMAtdTomato+ cells in the dental pulp increased in number after pulp exposure injury of αSMACreERT2/Ai9 transgenic mice.[42] The increased proliferation is seen even in areas away from the injury. In addition, α-SmatdTomato+ cells contributed to calcified reparative dentin bridge, suggesting their role in new odontoblast and dentin formation.[42] Similarly, NG2CreER; Rosa26-LacZ mice showed that perivascular NG2+ DPSCs can contribute to dentin formation upon in vivo injury.[79] However, the activation and differentiation of endogenous DPSCs in response to injury is a complex process influenced by various factors. These include the type of injury, its location, and severity. The age of the individual, as well as the difference in individuals and genders, can also affect the response of DPSCs to injury. Given the signaling molecules and growth factors present in the microenvironment can vary between individuals, in vivo experiments with the goal of investigating these differences would be more impactful to the development of new dental medicine and bone research.
DPSCs in pulp injury have great potential for future applications in regenerative medicine and dentistry. Researchers are studying the molecular and cellular mechanisms underlying the response of DPSCs to injury and the formation of reparative dentin. Supplementing these in vivo injury studies with scRNA analysis can additionally aid in further identifying DPSCs-specific markers, unique DPSCs subpopulations, and molecules that regulate DPSCs during development and dental injury repair. This knowledge could lead to the developing of new therapies for dental pulp regeneration, repair, and replacement.
In addition, the mouse tooth injury model has immense potential to contribute to the field of dentistry by offering insights into the mechanisms involved in tooth regeneration and repair. The surgical technique entails inducing a controlled injury to the tooth, which triggers the recruitment of DPSCs and immune cells and the development of new dentin and other tooth structures. Application of tooth injury models in transgenic reporter mice will allow postnatal tracing and the characterization of endogenous DPSCs under their natural environment. Results would therefore be more physiologically accurate, reproducible, and translatable to the clinical setting.
The mouse tooth injury models can be applied to the development of innovative dental materials and devices. Researchers have utilized the model to investigate the effectiveness of various regenerative therapies and biomaterials for repairing dental defects, such as enamel and pulpitis.[80,81] Furthermore, the model has the potential to aid in creating new techniques for restoring dental function and aesthetics, such as tissue engineering approaches for tooth replacement.[82,83]
In the future, further refinement and standardization of the mouse tooth injury model are required to increase the reproducibility and comparability of studies across various research groups. For example, the surgical technique could be improved by integrating advanced imaging techniques such as micro-computed tomography to enable more precise analysis of the injured tooth and surrounding tissues.[84,85] Further, intravital or in vivo imaging of the dental apparatus will enable longitudinal imaging of DPSCs at a subcellular resolution in live animals. The advancements in fiber optic technology and the innovation of new probes make in vivo imaging of endogenous DPSCs possible in the future.[64] Overall, studying DPSCs in the mouse tooth injury model has significant potential to contribute to the field of dental research and to aid in the development of new regenerative therapies and materials for dental repair and replacement.
Acknowledgments
This work was supported by the Bone Disease Program of Texas Award, the NIAMS of the National Institutes of Health under award numbers R61AR078073, 1R01AR072018 to D.P and T32DK060445 to L.O and Y.J. We thank M.E. Dickinson, J. Kirk in the BCM Optical Imaging and Vital Microscopy Core. The authors are grateful to Korean Society for Bone and Mineral Research (KSBMR) for the valuable invitation regarding this review.
Fig. 1
A schematic representation of the mouse lower jawbone (mandible) with a longitudinal section view. The sectioned area showcases the contact surface extending from the condyle head of the mandibular bone to the mandibular incisor tip. The mouse incisor is anatomically divided into 2 distinct parts: the crown, which constitutes the lower half, and the root, which comprises the upper half. Within the tooth structure, the incisor pulp (pink) occupies the internal portion of the tooth and originates from the cervical loop and extends extensively towards outside covered with hard tissue. Deep within the oral cavity, 3 molars are aligned in a sequential manner from front to back (from the right: 1st molar, 2nd molar, 3rd molar). An enlarged cross-section of the first molar in the right figure, providing additional detail and focusing specifically on this tooth structure.

Fig. 2
The endodontic Ellis system of dental trauma for dentin/pulp injury guideline. Based on the seriousness of injury on tooth surface, Ellis classified the tooth injury with 3 classes. Ellis Class I involves a complete fracture of the enamel with no dentin exposure. Ellis Class II is when the injury exposes the dentin. Ellis Class III are full-thickness fractures with pulp exposure and associated bleeding. Each Class was classified as shown in the figure based on the position of the injury line.
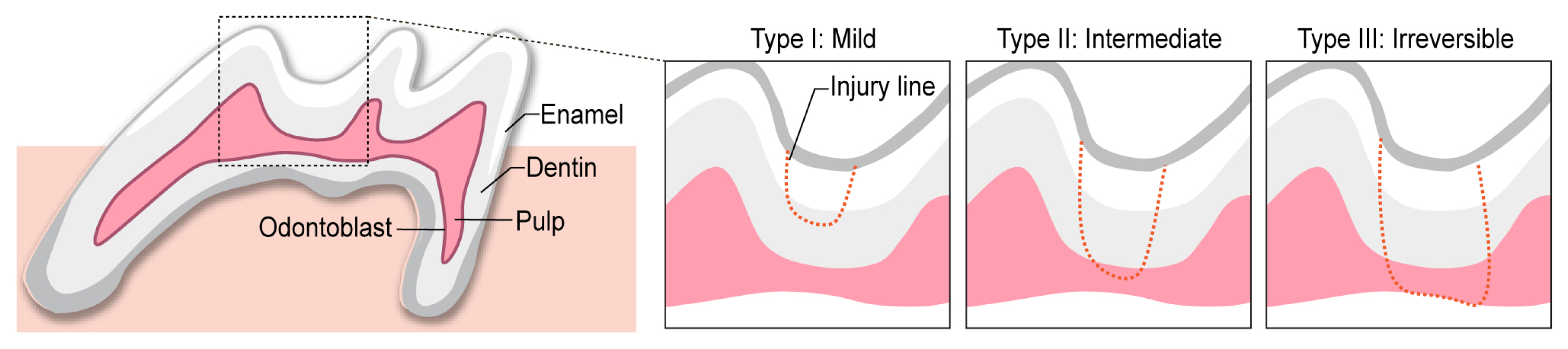
Fig. 3
Standardized mouse tooth injury method. In the cavity formation step, a controlled cavity is created by mechanically removing hard tissue at the targeted site using a precision instrument, such as a high-speed handpiece. Moving to the pulp opening step, a more extensive cavity is formed within the pulp tissue using a fine instrument, such as an endodontic file. Lastly, in the cavity sealing step, a suitable filling material is employed to effectively seal and occlude both the cavity created in the hard tissue and the opening formed within the pulp.
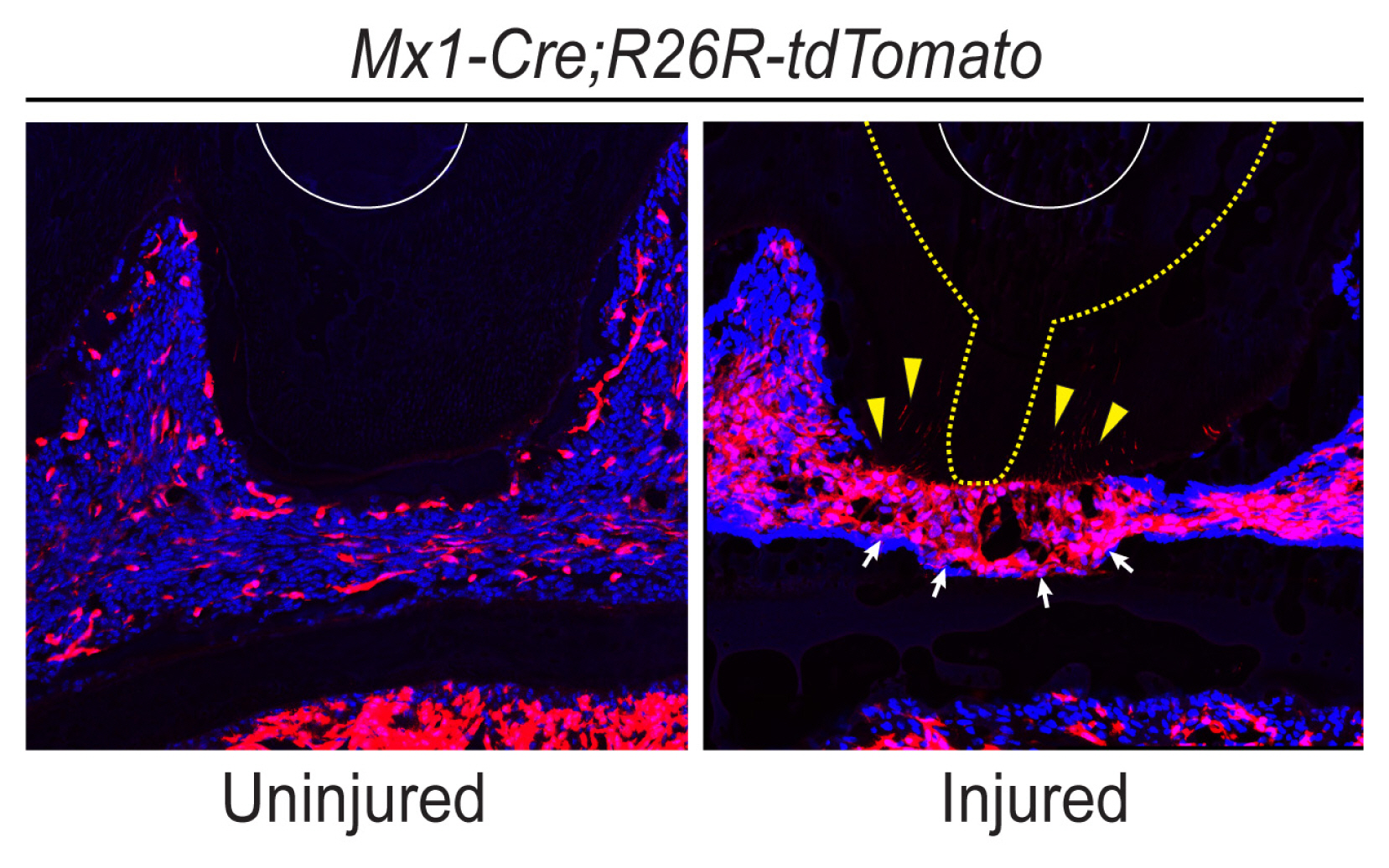
Fig. 4
To investigate the injury response applying new injury method using hand operated drill bit. In the experiment, genetically modified Mx1Cre/Tom+ mouse model was used, and it was designed to track the Mx1 gene, known as a mesenchymal stem/progenitor marker, to explore the injury response of stem/progenitor cells in pulp. To induce the injury, an initial cavity was created using a micro drill bit with a diameter of 0.25 mm. Subsequently, pulp opening was performed using a micro drill bit with a diameter of 0.10 mm. After a period of 2 weeks, the mice were sacrificed, and cryosection slides were analyzed using a confocal microscope. Compared to the uninjured model, the injured model exhibited increased proliferation of Mx1 cells in the pulp (white arrows). Additionally, some Mx1 expression was observed in the dentin area where the odontoblasts are located (yellow wedges). White line, enamel; yellow dotted line, injury line.
REFERENCES
1. Currey JD. The design of mineralised hard tissues for their mechanical functions. J Exp Biol 1999;202:3285-94. https://doi.org/10.1242/jeb.202.23.3285.


2. Gronthos S, Mankani M, Brahim J, et al. Postnatal human dental pulp stem cells (DPSCs) in vitro and in vivo. Proc Natl Acad Sci U S A 2000;97:13625-30. https://doi.org/10.1073/pnas.240309797.



3. He H, Yu J, Liu Y, et al. Effects of FGF2 and TGFbeta1 on the differentiation of human dental pulp stem cells in vitro. Cell Biol Int 2008;32:827-34. https://doi.org/10.1016/j.cellbi.2008.03.013.


4. Wang X, Sha XJ, Li GH, et al. Comparative characterization of stem cells from human exfoliated deciduous teeth and dental pulp stem cells. Arch Oral Biol 2012;57:1231-40. https://doi.org/10.1016/j.archoralbio.2012.02.014.


5. Kim S, Shin SJ, Song Y, et al. In vivo experiments with dental pulp stem cells for pulp-dentin complex regeneration. Mediators Inflamm 2015;2015:409347.https://doi.org/10.1155/2015/409347.



6. Aubeux D, Renard E, Pérez F, et al. Review of animal models to study pulp inflammation. Front Dent Med 2021;2:673552.https://doi.org/10.3389/fdmed.2021.673552.

7. Yu T, Klein OD. Molecular and cellular mechanisms of tooth development, homeostasis and repair. Development 2020;147:dev184754.https://doi.org/10.1242/dev.184754.



8. Galler KM, Weber M, Korkmaz Y, et al. Inflammatory response mechanisms of the dentine-pulp complex and the periapical tissues. Int J Mol Sci 2021;22:1480.https://doi.org/10.3390/ijms22031480.



9. Liu J, Yu F, Sun Y, et al. Concise reviews: characteristics and potential applications of human dental tissue-derived mesenchymal stem cells. Stem Cells 2015;33:627-38. https://doi.org/10.1002/stem.1909.


10. Li B, Ouchi T, Cao Y, et al. Dental-derived mesenchymal stem cells: state of the art. Front Cell Dev Biol 2021;9:654559.https://doi.org/10.3389/fcell.2021.654559.



11. Staniowski T, Zawadzka-Knefel A, Skośkiewicz-Malinowska K. Therapeutic potential of dental pulp stem cells according to different transplant types. Molecules 2021;26:7423.https://doi.org/10.3390/molecules26247423.



12. Anitua E, Troya M, Zalduendo M. Progress in the use of dental pulp stem cells in regenerative medicine. Cytotherapy 2018;20:479-98. https://doi.org/10.1016/j.jcyt.2017.12.011.


13. Gronthos S, Brahim J, Li W, et al. Stem cell properties of human dental pulp stem cells. J Dent Res 2002;81:531-5. https://doi.org/10.1177/154405910208100806.


14. Shahidi MK. Peripheral nerve glia as multipotent progenitors in craniofacial development [dissertation]. Stockholm, SE: Karolinska Institutet; 2015.
15. Hermans F, Hemeryck L, Lambrichts I, et al. Intertwined signaling pathways governing tooth development: a give-and-take between canonical wnt and shh. Front Cell Dev Biol 2021;9:758203.https://doi.org/10.3389/fcell.2021.758203.



16. Jing J, Feng J, Yuan Y, et al. Spatiotemporal single-cell regulatory atlas reveals neural crest lineage diversification and cellular function during tooth morphogenesis. Nat Commun 2022;13:4803.https://doi.org/10.1038/s41467-022-32490-y.



17. Huang GT, Yamaza T, Shea LD, et al. Stem/progenitor cell-mediated de novo regeneration of dental pulp with newly deposited continuous layer of dentin in an in vivo model. Tissue Eng Part A 2010;16:605-15. https://doi.org/10.1089/ten.TEA.2009.0518.



18. Lindroos B, Mäenpää K, Ylikomi T, et al. Characterisation of human dental stem cells and buccal mucosa fibroblasts. Biochem Biophys Res Commun 2008;368:329-35. https://doi.org/10.1016/j.bbrc.2008.01.081.


19. Shi S, Gronthos S. Perivascular niche of postnatal mesenchymal stem cells in human bone marrow and dental pulp. J Bone Miner Res 2003;18:696-704. https://doi.org/10.1359/jbmr.2003.18.4.696.


20. Dong Q, Wang Y, Mohabatpour F, et al. Dental pulp stem cells: Isolation, characterization, expansion, and odontoblast differentiation for tissue engineering. Methods Mol Biol 2019;1922:91-101. https://doi.org/10.1007/978-1-4939-9012-2_9.


21. Iezzi I, Cerqueni G, Licini C, et al. Dental pulp stem cells senescence and regenerative potential relationship. J Cell Physiol 2019;234:7186-97. https://doi.org/10.1002/jcp.27472.


22. Cao HL, Chung JH, Choung PH. Allogeneic fibrin clot for odontogenic/cementogenic differentiation of human dental mesenchymal stem cells. Tissue Eng Regen Med 2020;17:511-24. https://doi.org/10.1007/s13770-020-00279-z.



23. Liu GX, Ma S, Li Y, et al. Hsa-let-7c controls the committed differentiation of IGF-1-treated mesenchymal stem cells derived from dental pulps by targeting IGF-1R via the MAPK pathways. Exp Mol Med 2018;50:1-14. https://doi.org/10.1038/s12276-018-0048-7.



24. Liu M, Zhao L, Hu J, et al. Endothelial cells and endothelin-1 promote the odontogenic differentiation of dental pulp stem cells. Mol Med Rep 2018;18:893-901. https://doi.org/10.3892/mmr.2018.9033.



25. Oh HJ, Choung HW, Lee HK, et al. CPNE7, a preameloblast-derived factor, regulates odontoblastic differentiation of mesenchymal stem cells. Biomaterials 2015;37:208-17. https://doi.org/10.1016/j.biomaterials.2014.10.016.


26. Krivanek J, Soldatov RA, Kastriti ME, et al. Dental cell type atlas reveals stem and differentiated cell types in mouse and human teeth. Nat Commun 2020;11:4816.https://doi.org/10.1038/s41467-020-18512-7.



27. Seidel K, Marangoni P, Tang C, et al. Resolving stem and progenitor cells in the adult mouse incisor through gene co-expression analysis. Elife 2017;6:e24712.https://doi.org/10.7554/eLife.24712.



28. Zhao H, Feng J, Seidel K, et al. Secretion of shh by a neurovascular bundle niche supports mesenchymal stem cell homeostasis in the adult mouse incisor. Cell Stem Cell 2014;14:160-73. https://doi.org/10.1016/j.stem.2013.12.013.



29. Wang L, You X, Zhang L, et al. Mechanical regulation of bone remodeling. Bone Res 2022;10:16.https://doi.org/10.1038/s41413-022-00190-4.



30. Bayarsaihan D, Enkhmandakh B, Vijaykumar A, et al. Single-cell transcriptome analysis defines mesenchymal stromal cells in the mouse incisor dental pulp. Gene Expr Patterns 2022;43:119228.https://doi.org/10.1016/j.gep.2021.119228.


31. Pagella P, de Vargas Roditi L, Stadlinger B, et al. A single-cell atlas of human teeth. iScience 2021;24:102405.https://doi.org/10.1016/j.isci.2021.102405.



32. Mortada I, Mortada R. Dental pulp stem cells and osteogenesis: an update. Cytotechnology 2018;70:1479-86. https://doi.org/10.1007/s10616-018-0225-5.



33. Li J, Parada C, Chai Y. Cellular and molecular mechanisms of tooth root development. Development 2017;144:374-84. https://doi.org/10.1242/dev.137216.



34. Ballini A, Cantore S, Scacco S, et al. A comparative study on different stemness gene expression between dental pulp stem cells vs. dental bud stem cells. Eur Rev Med Pharmacol Sci 2019;23:1626-33. https://doi.org/10.26355/eurrev_201902_17122.


35. Huang CE, Hu FW, Yu CH, et al. Concurrent expression of Oct4 and Nanog maintains mesenchymal stem-like property of human dental pulp cells. Int J Mol Sci 2014;15:18623-39. https://doi.org/10.3390/ijms151018623.



36. Tao H, Lin H, Sun Z, et al. Klf4 promotes dentinogenesis and odontoblastic differentiation via modulation of TGF-β signaling pathway and interaction with histone acetylation. J Bone Miner Res 2019;34:1502-16. https://doi.org/10.1002/jbmr.3716.



37. Liu Y, Gan L, Cui DX, et al. Epigenetic regulation of dental pulp stem cells and its potential in regenerative endodontics. World J Stem Cells 2021;13:1647-66. https://doi.org/10.4252/wjsc.v13.i11.1647.



38. Casagrande L, Cordeiro MM, Nör SA, et al. Dental pulp stem cells in regenerative dentistry. Odontology 2011;99:1-7. https://doi.org/10.1007/s10266-010-0154-z.


39. Piglionico SS, Pons C, Romieu O, et al. In vitro, ex vivo, and in vivo models for dental pulp regeneration. J Mater Sci Mater Med 2023;34:15.https://doi.org/10.1007/s10856-023-06718-2.



40. Tatullo M, Marrelli M, Shakesheff KM, et al. Dental pulp stem cells: function, isolation and applications in regenerative medicine. J Tissue Eng Regen Med 2015;9:1205-16. https://doi.org/10.1002/term.1899.


41. Babb R, Chandrasekaran D, Carvalho Moreno Neves V, et al. Axin2-expressing cells differentiate into reparative odontoblasts via autocrine Wnt/β-catenin signaling in response to tooth damage. Sci Rep 2017;7:3102.https://doi.org/10.1038/s41598-017-03145-6.



42. Vidovic I, Banerjee A, Fatahi R, et al. αSMA-expressing perivascular cells represent dental pulp progenitors in vivo. J Dent Res 2017;96:323-30. https://doi.org/10.1177/0022034516678208.



43. Nagata M, Ono N, Ono W. Unveiling diversity of stem cells in dental pulp and apical papilla using mouse genetic models: a literature review. Cell Tissue Res 2021;383:603-16. https://doi.org/10.1007/s00441-020-03271-0.



44. Oka S, Oka K, Xu X, et al. Cell autonomous requirement for TGF-beta signaling during odontoblast differentiation and dentin matrix formation. Mech Dev 2007;124:409-15. https://doi.org/10.1016/j.mod.2007.02.003.



45. Feng J, Jing J, Li J, et al. BMP signaling orchestrates a transcriptional network to control the fate of mesenchymal stem cells in mice. Development 2017;144:2560-9. https://doi.org/10.1242/dev.150136.



46. Mitchell JM, Hicklin DM, Doughty PM, et al. The Prx1 homeobox gene is critical for molar tooth morphogenesis. J Dent Res 2006;85:888-93. https://doi.org/10.1177/154405910608501003.



47. Esposito A, Wang L, Li T, et al. Role of Prx1-expressing skeletal cells and Prx1-expression in fracture repair. Bone 2020;139:115521.https://doi.org/10.1016/j.bone.2020.115521.



48. Solidum JGN, Jeong Y, Heralde F 3rd, et al. Differential regulation of skeletal stem/progenitor cells in distinct skeletal compartments. Front Physiol 2023;14:1137063.https://doi.org/10.3389/fphys.2023.1137063.



49. Wilk K, Yeh SA, Mortensen LJ, et al. Postnatal calvarial skeletal stem cells expressing PRX1 reside exclusively in the calvarial sutures and are required for bone regeneration. Stem Cell Reports 2017;8:933-46. https://doi.org/10.1016/j.stemcr.2017.03.002.



50. Park D, Spencer JA, Koh BI, et al. Endogenous bone marrow MSCs are dynamic, fate-restricted participants in bone maintenance and regeneration. Cell Stem Cell 2012;10:259-72. https://doi.org/10.1016/j.stem.2012.02.003.



51. Andreasen JO, Ahrensburg SS. History of the dental trauma guide. Dent Traumatol 2012;28:336-44. https://doi.org/10.1111/j.1600-9657.2011.01097.x.


52. Byers MR, Närhi MV. Dental injury models: experimental tools for understanding neuroinflammatory interactions and polymodal nociceptor functions. Crit Rev Oral Biol Med 1999;10:4-39. https://doi.org/10.1177/10454411990100010101.


53. Marchesan J, Girnary MS, Jing L, et al. An experimental murine model to study periodontitis. Nat Protoc 2018;13:2247-67. https://doi.org/10.1038/s41596-018-0035-4.



54. Kuraji R, Hashimoto S, Ito H, et al. Development and use of a mouth gag for oral experiments in rats. Arch Oral Biol 2019;98:68-74. https://doi.org/10.1016/j.archoralbio.2018.11.008.


55. Athos J, Storm DR. High precision stereotaxic surgery in mice. Curr Protoc Neurosci 2001 Appendix 4:Appendix 4A. https://doi.org/10.1002/0471142301.nsa04as14.


56. Chung MK, Lee J, Duraes G, et al. Lipopolysaccharide-induced pulpitis up-regulates TRPV1 in trigeminal ganglia. J Dent Res 2011;90:1103-7. https://doi.org/10.1177/0022034511413284.



57. Cunningham MG, McKay RD. A hypothermic miniaturized stereotaxic instrument for surgery in newborn rats. J Neurosci Methods 1993;47:105-14. https://doi.org/10.1016/0165-0270(93)90026-n.


58. Kimberly CL, Byers MR. Inflammation of rat molar pulp and periodontium causes increased calcitonin gene-related peptide and axonal sprouting. Anat Rec 1988;222:289-300. https://doi.org/10.1002/ar.1092220310.


59. Neves VC, Babb R, Chandrasekaran D, et al. Promotion of natural tooth repair by small molecule GSK3 antagonists. Sci Rep 2017;7:39654.https://doi.org/10.1038/srep39654.



60. Walker JV, Zhuang H, Singer D, et al. Transit amplifying cells coordinate mouse incisor mesenchymal stem cell activation. Nat Commun 2019;10:3596.https://doi.org/10.1038/s41467-019-11611-0.



61. Zaugg LK, Banu A, Walther AR, et al. Translation approach for dentine regeneration using GSK-3 antagonists. J Dent Res 2020;99:544-51. https://doi.org/10.1177/0022034520908593.



62. Dao V, Renjen R, Prasad HS, et al. Cementum, pulp, periodontal ligament, and bone response after direct injury with orthodontic anchorage screws: a histomorphologic study in an animal model. J Oral Maxillofac Surg 2009;67:2440-5. https://doi.org/10.1016/j.joms.2009.04.138.


63. Hague BA, Honnas CM. Traumatic dental disease and soft tissue injuries of the oral cavity. Vet Clin North Am Equine Pract 1998;14:333-47. https://doi.org/10.1016/s0749-0739(17)30201-8.


64. Yang D, Ortinau L, Jeong Y, et al. Advances and challenges in intravital imaging of craniofacial and dental progenitor cells. Genesis 2022;60:e23498.https://doi.org/10.1002/dvg.23498.



65. Zhang W, Ju J. Odontoblast-targeted Bcl-2 overexpression promotes dentine damage repair. Arch Oral Biol 2012;57:285-92. https://doi.org/10.1016/j.archoralbio.2011.08.022.



66. Zhao Y, Yuan X, Liu B, et al. Wnt-responsive odontoblasts secrete new dentin after superficial tooth injury. J Dent Res 2018;97:1047-54. https://doi.org/10.1177/0022034518763151.



67. Simon S, Cooper P, Smith A, et al. Evaluation of a new laboratory model for pulp healing: preliminary study. Int Endod J 2008;41:781-90. https://doi.org/10.1111/j.1365-2591.2008.01433.x.


68. Vidovic-Zdrilic I, Vining KH, Vijaykumar A, et al. FGF2 enhances odontoblast differentiation by αSMA(+) progenitors in vivo. J Dent Res 2018;97:1170-7. https://doi.org/10.1177/0022034518769827.



69. Hegde VS, Khatavkar RA. A new dimension to conservative dentistry: air abrasion. J Conserv Dent 2010;13:4-8. https://doi.org/10.4103/0972-0707.62632.



70. Sulewski JG. Chapter-12 Air abrasion: Background and cavity preparation. In: Graeber JJ, editors. Microinvasive dentistry: Clinical strategies and tools. New Delhi, IN: Jaypee Brothers Medical Publishers; 2021. p.99. -106.
71. Kimura Y, Wilder-Smith P, Matsumoto K. Lasers in endodontics: a review. Int Endod J 2000;33:173-85. https://doi.org/10.1046/j.1365-2591.2000.00280.x.


72. Kitamura C, Nishihara T, Terashita M, et al. Regeneration approaches for dental pulp and periapical tissues with growth factors, biomaterials, and laser irradiation. Polymers (Basel) 2011;3:1776-93. https://doi.org/10.3390/polym3041776.

73. Lea SC, Felver B, Landini G, et al. Ultrasonic scaler oscillations and tooth-surface defects. J Dent Res 2009;88:229-34. https://doi.org/10.1177/0022034508330267.


74. Lefkowitz W, Robinson HBG, Postle HH. Pulp response to cavity preparation. J Prosthet Dent 1958;8:315-24. https://doi.org/10.1016/0022-3913(58)90164-1.

75. Elkhazindar MM, Welbury RR. Enamel microabrasion. Dent Update 2000;27:194-6. https://doi.org/10.12968/denu.2000.27.4.194.


76. Pini NI, Sundfeld-Neto D, Aguiar FH, et al. Enamel microabrasion: an overview of clinical and scientific considerations. World J Clin Cases 2015;3:34-41. https://doi.org/10.12998/wjcc.v3.i1.34.



77. Angelova Volponi A, Zaugg LK, Neves V, et al. Tooth repair and regeneration. Curr Oral Health Rep 2018;5:295-303. https://doi.org/10.1007/s40496-018-0196-9.



78. Neves VCM, Sharpe PT. Regulation of reactionary dentine formation. J Dent Res 2018;97:416-22. https://doi.org/10.1177/0022034517743431.


79. Feng J, Mantesso A, De Bari C, et al. Dual origin of mesenchymal stem cells contributing to organ growth and repair. Proc Natl Acad Sci U S A 2011;108:6503-8. https://doi.org/10.1073/pnas.1015449108.



80. Long Y, Liu S, Zhu L, et al. Evaluation of pulp response to novel bioactive glass pulp capping materials. J Endod 2017;43:1647-50. https://doi.org/10.1016/j.joen.2017.03.011.


81. Shuai Y, Ma Y, Guo T, et al. Dental stem cells and tooth regeneration. Adv Exp Med Biol 2018;1107:41-52. https://doi.org/10.1007/5584_2018_252.


82. Morsczeck C, Reichert TE. Dental stem cells in tooth regeneration and repair in the future. Expert Opin Biol Ther 2018;18:187-96. https://doi.org/10.1080/14712598.2018.1402004.


83. Xiao L, Nasu M. From regenerative dentistry to regenerative medicine: progress, challenges, and potential applications of oral stem cells. Stem Cells Cloning 2014;7:89-99. https://doi.org/10.2147/sccaa.S51009.



84. Huang GT. Pulp and dentin tissue engineering and regeneration: current progress. Regen Med 2009;4:697-707. https://doi.org/10.2217/rme.09.45.



- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 2,040 View
- 37 Download
- ORCID iDs
-
Dongwook Yang

https://orcid.org/0000-0002-9030-597XJea Giezl Niedo Solidum

https://orcid.org/0000-0002-7161-2106Dongsu Park

https://orcid.org/0000-0002-2570-3250 - Related articles




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print