|
 |
| jbm > Volume 29(4); 2022 > Article |
|
Abstract
Background
Methods
Results
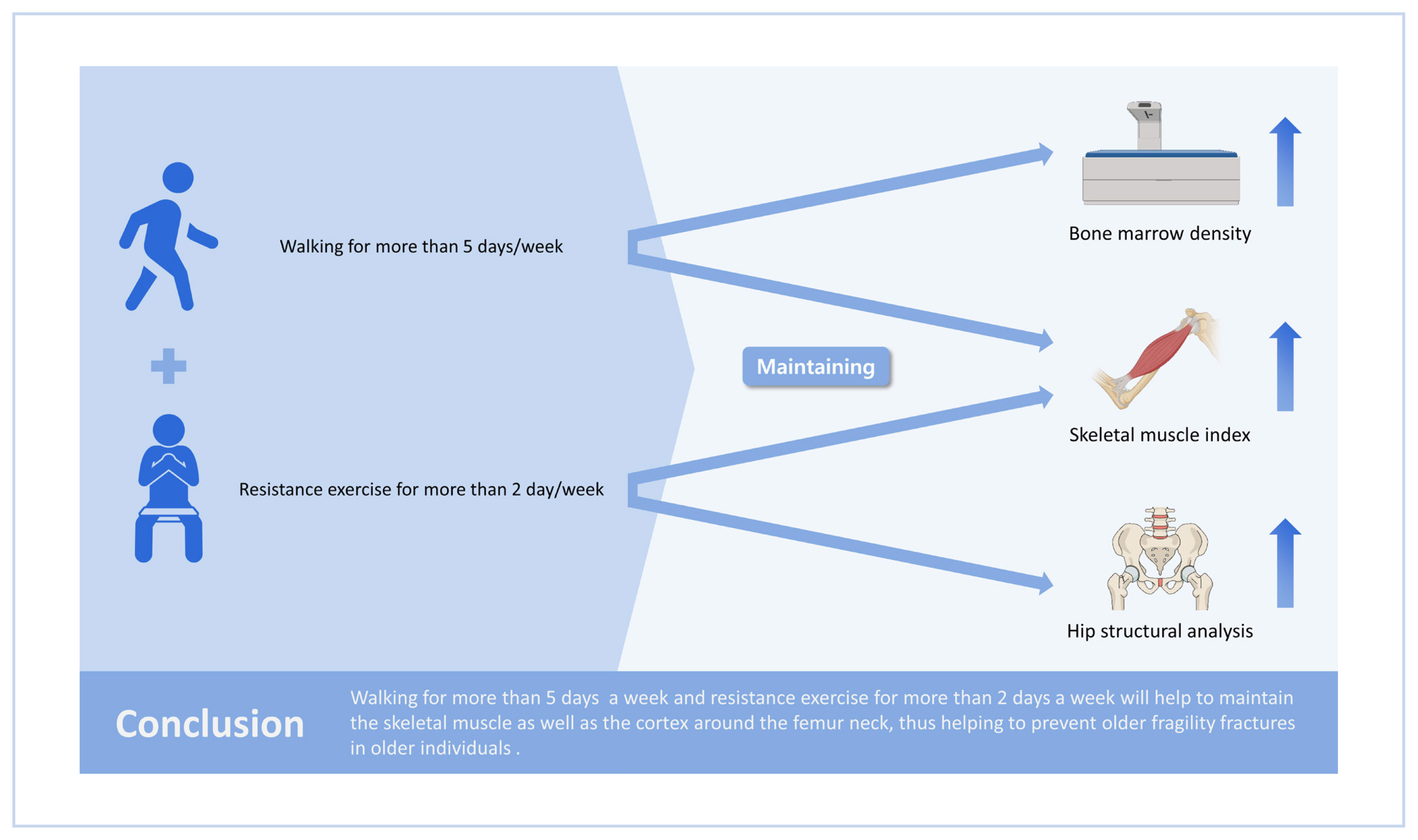
Conclusions
DECLARATIONS
Funding
This research was supported by a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (Grant number: HI22C0494).
Ethics approval and consent to participate
Data from the 2008 Korean National Health and Nutrition Examination Survey (KNHANES), bearing the approval number 2008-04EXP-01-C, was reviewed and approved by the Institutional Review Board of the Korea Centers for Disease Control and Prevention (K-CDC) and all participants provided written informed consent.
Fig. 1
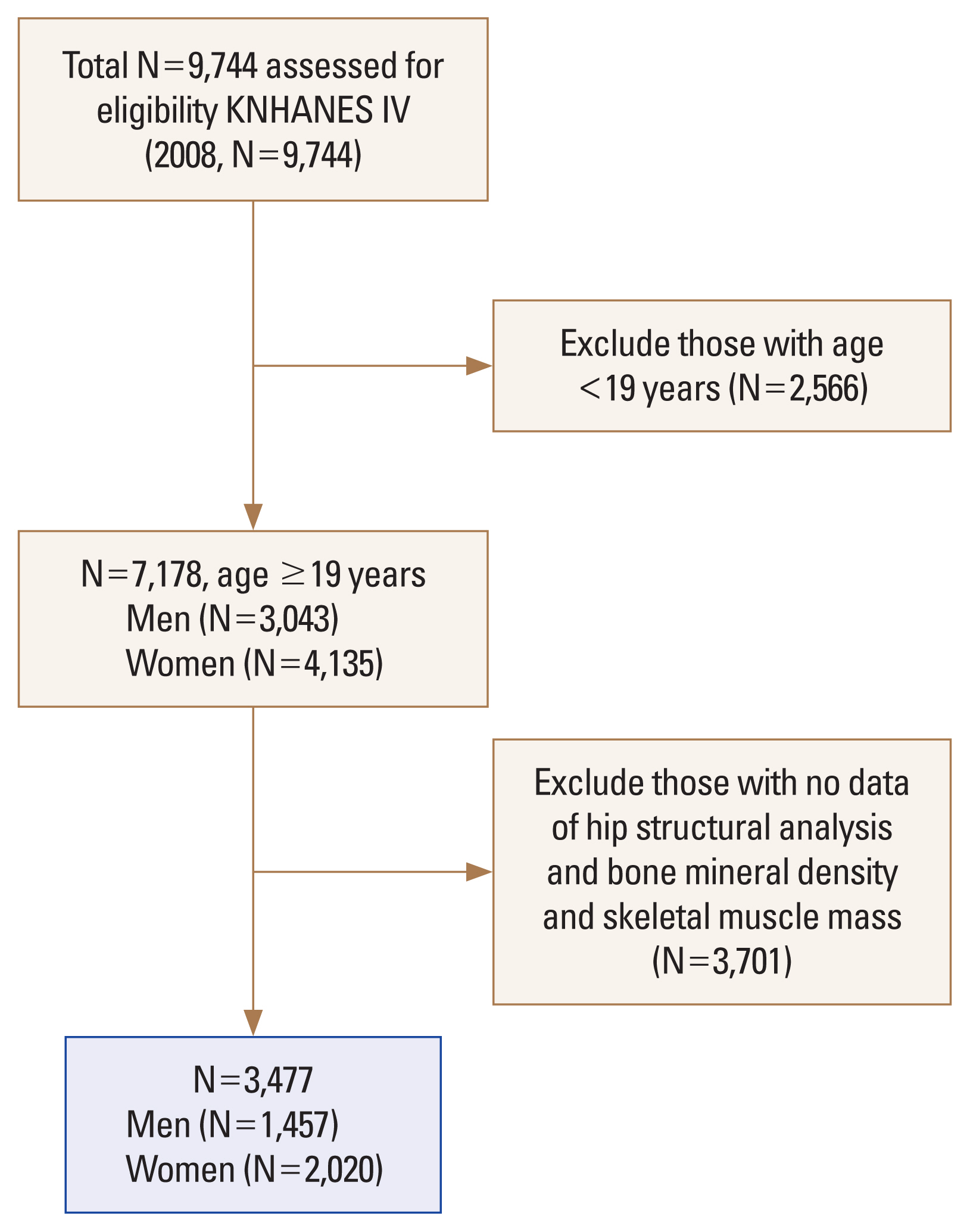
Table 1
| Variables | Age <65 (N=2,730) | Age ≥65 (N=747) | P-valuee) |
|---|---|---|---|
| Age (yr) | 42.4±12.2 | 71.8±5.3 | <0.0001 |
|
|
|||
| Female | 1,567 (57.4) | 453 (60.6) | <0.0001 |
|
|
|||
| Height (cm) | 163.4±8.7 | 156.1±8.9 | <0.0001 |
|
|
|||
| Weight (kg) | 62.8±11.3 | 57.3±9.9 | 0.889 |
|
|
|||
| BMI (kg/m2) | 23.4±3.3 | 23.4±3.2 | <0.0001 |
|
|
|||
| Incomea) | 645 (24.0) | 176 (23.6) | 0.716 |
|
|
|||
| Educationb) | 2,269 (83.1) | 167 (22.4) | <0.0001 |
|
|
|||
| Osteoporosis | 97 (3.6) | 263 (35.2) | <0.0001 |
|
|
|||
| Energy intake (kcal/day) | 1,902.2±804.5 | 1,565.1±603.4 | <0.001 |
|
|
|||
| Muscle-strengthening activityc) | 769 (28.2) | 85 (11.4) | <0.001 |
|
|
|||
| Walking activityd) | 1,339 (49.0) | 364 (48.7) | 0.877 |
|
|
|||
| Physical activity | <0.001 | ||
| Non activity | 1,047 (38.4) | 347 (46.5) | |
| Only waking | 914 (33.5) | 315 (42.2) | |
| Only muscle activity | 344 (12.6) | 36 (4.8) | |
| Walking and muscle activity | 425 (15.6) | 49 (6.6) | |
Table 2
Table 3
Table 4
| Variables | Total age <65 | Total age ≥65 | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|||||||||
| Non activity (N=1,047) | Only walking (N=914) | Only muscle activity (N=344) | Walking and muscle activity (N=425) | P-value | Non activity (N=347) | Only walking (N=315) | Only uscle activity (N=36) | Walking and muscle activity (N=49) | P-value | |
| CSA of femur neck | 2.901±0.025 | 2.894±0.026 | 2.924±0.041 | 2.932±0.037 | 0.764 | 2.868±0.043 | 2.841±0.042 | 2.865±0.111 | 3.100±0.093 | 0.093 |
|
|
||||||||||
| Cortical thickness of femur neck | 0.174±0.001 | 0.173±0.001 | 0.174±0.002 | 0.175±0.002 | 0.895 | 0.170±0.002 | 0.170±0.002 | 0.169±0.006 | 0.177±0.005 | 0.630 |
|
|
||||||||||
| CSA of intertrochanter area | 4.717±0.044 | 4.727±0.045 | 4.822±0.071 | 4.833±0.064 | 0.211 | 4.660±0.074 | 4.674±0.073 | 4.456±0.193 | 4.904±0.162 | 0.338 |
|
|
||||||||||
| Cortical thickness of intertrochanter area | 0.392±0.004 | 0.394±0.004 | 0.402±0.006 | 0.401±0.005 | 0.215 | 0.389±0.006 | 0.391±0.006 | 0.366±0.016 | 0.400±0.014 | 0.424 |
|
|
||||||||||
| BMD (g/cm3) of femur neck | 0.738±0.005a) | 0.741±0.005a) | 0.764±0.008b) | 0.768±0.007b) | <0.001 | 0.619±0.007a) | 0.640±0.007a) | 0.646±0.019a) | 0.695±0.016b) | <0.001 |
|
|
||||||||||
| BMD (g/cm3) of intertrochanter area | 1.063±0.006a) | 1.072±0.006a) | 1.098±0.009b) | 1.103±0.008b) | <0.001 | 0.939±0.010a) | 0.974±0.010a) | 0.960±0.025a) | 1.059±0.021b) | <0.001 |
|
|
||||||||||
| BMD (g/cm3) of lumbar spine | 0.923±0.005 | 0.925±0.005 | 0.938±0.008 | 0.935±0.008 | 0.213 | 0.827±0.010a) | 0.851±0.010a) | 0.822±0.028a) | 0.909±0.022b) | 0.004 |
|
|
||||||||||
| SMI (kg/m2) | 6.757±0.037a) | 6.897±0.038a) | 7.410±0.061b) | 7.346±0.055b) | <0.001 | 6.687±0.056a) | 6.921±0.055a) | 7.158±0.146a) | 7.345±0.121b) | <0.001 |
REFERENCES
- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 3,427 View
- 100 Download
- ORCID iDs
-
Sangyeob Lee

https://orcid.org/0000-0001-8024-1135Ji-Seok Kim

https://orcid.org/0000-0002-3023-1999Ki-Soo Park

https://orcid.org/0000-0001-5571-3639Kyung-Wan Baek

https://orcid.org/0000-0002-8445-3773Jun-Il Yoo

https://orcid.org/0000-0002-3575-4123 - Related articles




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print