Association between Bone Mineral Density and Coronary Atherosclerotic Plaque According to Plaque Composition: Registry for the Women Health Cohort for Bone, Breast, and Coronary Artery Disease Study
Article information
Abstract
Background
Although biological links are unclear, low bone density and atherosclerosis are inversely associated. This study evaluated the association between bone mineral density (BMD) and coronary computed tomographic angiography (CCTA) findings, including coronary artery calcification (CAC) score and the presence, extent, and composition of coronary atherosclerotic plaque (CAP) in asymptomatic women.
Methods
A symptomatic women aged ≥40 years (N=2, 100; median age, 52 years; range, 40–80 years) were selected from a retrospective observational cohort and stratified into normal, osteopenia, and osteoporosis groups according to BMD T-score grades. We evaluated CAC score and assessed the presence, extent, and stenosis severity of CAP on CCTA. Additionally, CAP was categorized as calcified, mixed, or non-calcified according to calcified component valiums (>130 Hounsfield units).
Results
Osteopenia and osteoporosis were found in 28.8% and 5.3% of participants, respectively. CAC score and CAC severity significantly increased with decreased BMD grades (from normal to osteoporosis). The presence of CAP (overall, 15.6%; normal, 12.6%; osteopenia, 20.2%; osteoporosis, 28.8%; P<0.001) and number of segments with CAP significantly increased with decreased BMD grades. Furthermore, the number of segments with calcified or mixed plaques, excluding non-calcified plaques, increased with decreased BMD grades. Although most associations were attenuated or disappeared after adjusting for age and other covariates, calcified plaques showed a strong and age-independent association with BMD grades.
Conclusions
The presence and severity of CAC and CAP were significantly associated with BMD severity in asymptomatic women, particularly for the presence of calcified plaques. Further studies are required to determine the association between vascular calcification and bone health status.
INTRODUCTION
Osteoporosis and atherosclerosis are representative diseases that occur with aging in the bone and vasculature, respectively, and have been acknowledged as major health burdens with the aging of society.[1,2] Many epidemiologic findings suggest potential links between osteoporosis and atherosclerosis, demonstrating an inverse relationship between bone mineral density (BMD) values and parameters related to atherosclerosis.[3,4] However, the biological mechanisms remain unclear, and controversies still exist regarding the association between atherosclerosis and osteoporosis.[5]
The pathogeneses of osteoporosis and atherosclerosis are very complicated.[6–8] Osteoporosis, generally defined as low BMD, is caused by a variety of complex mechanisms, including sex hormone deprivation, chronic inflammation, oxidative stress accumulation, and calcium balance disturbance.[6] As in osteoporosis, various risk factors and molecular mechanisms are involved in atherosclerosis, and vascular calcification is one of the major features of atherosclerosis.[9,10] Coronary atherosclerotic plaque (CAP), an occlusive lesion of the arterial lumen, is a representative parameter of atherosclerosis, and is a marker of greater risk for future cardiovascular events.[11,12] The aging process per se, renal insufficiency, diabetes, or altered calcium balance may accelerate vascular calcification and contribute to the progression of atherosclerosis.[10] Furthermore, beyond vascular calcification, other diverse mechanisms, such as inflammation, cell death, and lipid oxidation, involve plaque formation in atherosclerosis processes.[10,13] CAP can be classified according to their calcium composition into calcified, partially calcified (mixed), and non-calcified plaques.[14] The plaque composition is determined according to the main pathophysiology contributing to plaque formation and is closely related to the risk of future cardiovascular events.[15]
Considering the changes in plaque composition during the progression of coronary atherosclerosis, a better understanding of the associations between plaque composition and BMD values may help clarify the biological basis underlying the link between bone and vessel. Therefore, in this study, we investigated plaque presence, extent, and composition according to BMD values in healthy Korean women.
METHODS
1. Study participants and design
The BBC study (Women Health Registry Study for Bone, Breast, and Coronary Artery Disease) was a cross-sectional study comprising consecutive self-referred women aged ≥40 years who underwent digital mammography, dual energy X-ray absorptiometry (DXA), and coronary computed tomographic angiography (CCTA), as part of a general health evaluation between March 2011 and February 2013. Among 2,113 women who underwent all 3 tests on the same day, we excluded women with a history of myocardial infarction or coronary revascularization or a history of breast surgery or intervention. The women treated with anti-osteoporotic medications including bisphosphonates or selective estrogen receptor modulator were also excluded. Although our exclusion criteria also included poor CCTA image quality and renal dysfunction with serum creatinine >1.4 mg/dL, none of the study participants demonstrated these features. Therefore, 2,100 women remained in the final analysis. The study design and primary study findings have been previously published.[16] The study was conducted in accordance with the Declaration of Helsinki and with Institutional Review Board approval.
2. BMD
Lumbar spine BMD was measured by certified radiological technologists using a single DXA scanner (GE Lunar, Madison, WI, USA). The entire lumbar spine was scanned in the posteroanterior view, and the BMD at the lumbar spine was calculated for the first to fourth vertebrae using densitometric software. Normal BMD was defined as a BMD T-score higher than −1.0, osteopenia as a BMD T-score less than −1.0 and higher than −2.5, and osteoporosis as a BMD T-score below −2.5, according to World Health Organization criteria.[17] T-scores were calculated using the reference ranges for Asian populations provided by the manufacturer. The coefficients of variation for DXA measurements for both lumbar and hip are <2% for all measures.
3. CCTA acquisition and analysis
Unenhanced and contrast-enhanced computed tomography (CT) angiography was performed using a 64-detector row CT scanner (Brilliance 64; Philips Medical Systems, Best, the Netherlands), in accordance with established guidelines [18] and institutional protocols at the time of the scan. CCTA images were transferred to an offline 3-dimensional workstation and independently analyzed by a cardiac radiologist with more than 10 years of experience, blinded to the clinical information, mammography, and DXA results. The coronary artery calcification (CAC) score was measured using the Agatston scoring system,[19] and the presence of CAC was defined as a CAC score >0. The CAC score was graded as follows: 0, 1 to 99, 100 to 399, and ≥400. CAP presence and composition were evaluated by a per-segment analysis, according to the modified American Heart Association 15-segment criteria.[20,21] CAP was defined as the presence of any discernible atherosclerotic plaque lesion >1 mm2 that could be discriminated from the coronary artery in at least two independent image planes.[16,22] Plaque composition was classified as non-calcified (<30% calcified plaque volume), partially calcified (30%–70%), or calcified (>70%) according to the calcified component (>130 Hounsfield units).[23]
4. Statistical analysis
All statistical analyses were performed using STATA 15.0 software (Stata Corp., College Station, TX, USA). Continuous variables are expressed as the mean±standard deviation, and categorical variables are expressed as proportions. Quantitative data were compared using the Student’s t-test, χ2 test, or Fisher’s exact test, as appropriate. Study participants were categorized into 3 groups according to their lumbar spine BMD T-score, with higher than −1.0 in the normal group, less than −1.0 and higher than −2.5 in the osteopenia group, and less than −2.5 in the osteoporosis group. Because of the skewed distribution of the CAC score, the log-transformed CAC score (ln [CAC score +1]) was compared between each BMD group. The addition of 1 to the CAC score before the logarithmic transformation allowed us to include all patients with a CAC score of zero. The scores and grades for breast arterial calcification (BAC) were evaluated as previously described.[16] Comparisons in BAC and CAC scores or numbers of segments with CAP among BMD T-score groups were performed by ANOVA and ANCOVA with adjustment for age and other covariates. The number of patients with any CAP and number of segments with non-calcified, partially calcified, and calcified plaques were compared among groups by linear association. For all analyses, a 2-sided P-value of less than 0.05 was considered to represent a statistically significant difference.
RESULTS
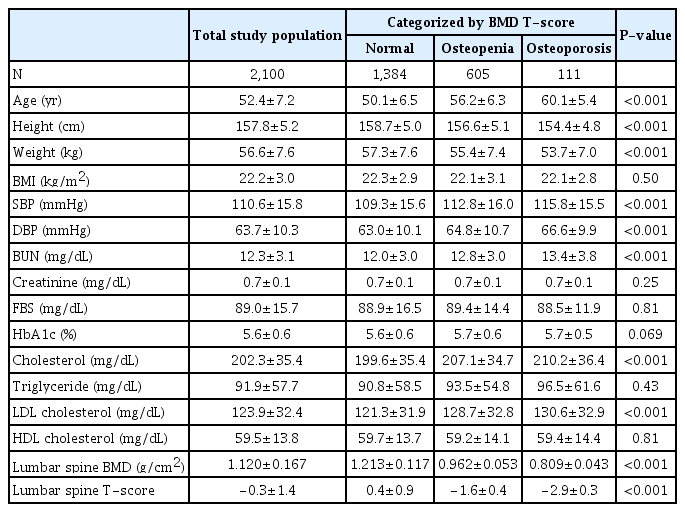
Table 1 presents the baseline characteristics of the study participants and 3 BMD groups according to the BMD T-scores. The mean age was 52.4 years and ranged from 40 to 80 years, and the mean body mass index was 22.2 kg/m2. Among the total study population, 605 of 2,100 (28.8%) participants had osteopenia, and 111 of 2,100 (5.3%) had osteoporosis. With decreased BMD grade (from normal to osteoporosis), the mean age increased, height and weight decreased, systolic blood pressure and diastolic blood pressure increased, and the levels of blood urea nitrogen and total cholesterol increased.
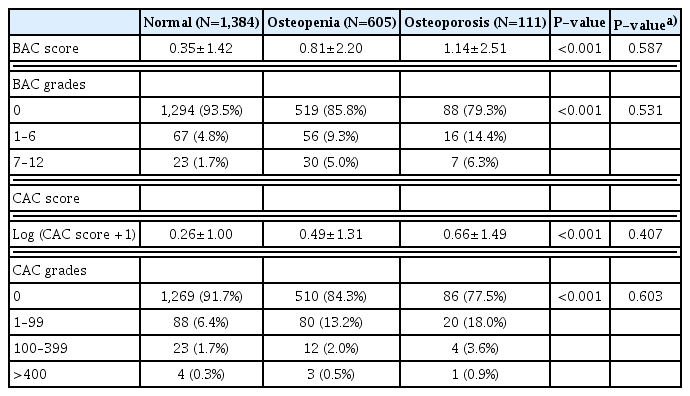
The BAC and CAC scores according to BMD T-score groups are shown in Table 2. With decreased BMD grade, the BAC score and proportion of participants with higher BAC scores increased (P<0.001 for both). Similarly, log-CAC scores and the proportion of participants with higher CAC scores were also increased with decreased BMD grades (Table 2). However, the significant differences in BAC and CAC scores among BMD groups disappeared after adjusting for age.
We further compared the proportion of participants with any CAP and the presence of each plaque compositional category across normal, osteopenia, and osteoporosis groups (Fig. 1). There was a significant increasing trend in the proportion of participants with any CAP with decreased BMD grade (normal, 12.57%; osteopenia, 20.17%; and osteoporosis, 28.83%; P<0.001) (Fig. 1A). Furthermore, the proportion of women with calcified or mixed plaque was significantly increased in the osteopenia and osteoporosis groups compared to that in the normal group (7.23%, 12.4%, and 18.02% for calcified plaque, and 2.1%, 4.13%, and 6.31% for mixed plaque, respectively; P<0.001) (Fig. 1B–C). However, the proportion of women with non-calcified plaques did not differ across BMD grades (Fig. 1D).

The proportion of women with CAP (any, calcified, partially calcified, or non-calcified plaque) in each BMD group. (A) Proportion of women with any CAP. (B) Proportion of women with non-calcified plaque. (C) Proportion of women with partially calcified (mixed) plaque. (D) Proportion of women with calcified plaque. BMD, bone mineral density; CAP, coronary atherosclerotic plaque.
The extent of CAP, evaluated as the number of segments with atherosclerotic plaques, overall and for each plaque compositional category, was also compared across BMD groups (Table 3). The number of segments with any CAP significantly increased with decreased BMD grade, suggesting more extensive CAD in women with lower BMD T-scores. However, these differences were not statistically significant after adjusting for age alone or conventional confounders. Further, the number of segments with calcified plaque was greater in the osteopenia and osteoporosis groups than in the normal group. Although these differences were attenuated after adjusting for age and other covariates, they remained significant (normal, 0.13±0.64; osteopenia, 0.22±0.73; osteoporosis, 0.25±0.65; P<0.05). Although the number of segments with partially calcified plaque was also increased in the osteopenia and osteoporosis groups compared to that in the normal group, the differences did not remain significant after adjusting for age and other covariates. In addition, the number of segments with non-calcified plaques did not significantly differ among the BMD groups.
DISCUSSION
In the present study, we tested the hypothesis that there is a significant association between atherosclerosis and osteoporosis, and that plaque composition may affect the potential associations between low bone density and atherosclerosis. The results of the present study revealed that there were significant associations between CAC or CAP and low bone density, but these were mostly age-dependent. However, calcified plaque showed a stronger and age-independent association with low bone density compared to that mixed or non-calcified plaques. Our findings suggest a potential link between low bone density and atherosclerosis, particularly for calcified plaque; accordingly, the specific pathogenesis that leads to calcified plaque formation might be closely related to the development and progression of low bone mass.
Bone is a composite of viable bone cells and an extracellular matrix, which mainly consists of a mineral matrix of calcium and phosphorus.[24] Diverse risk factors, including aging and estrogen deprivation, cause bone cell apoptosis and loss of mineral matrix in bone tissue, leading to osteopenia and osteoporosis.[25,26] Atherosclerosis is also a consequence of complicated biological processes.[8,13] Plaque formation in the vascular wall is an early and significant sign of future atherosclerotic events.[27] The major histologic features of atherosclerotic plaque are calcium deposition in the vasculature, inflammatory cell infiltration, and lipid accumulation, and the plaque can be characterized as calcified, non-calcified, or mixed.[9,14]
Based on several epidemiologic studies, it has been suggested that there is a potential association between atherosclerosis and osteoporosis; patients with atherosclerosis have a higher risk of osteoporosis and fractures, and vice versa.[3,28,29] Furthermore, longitudinal studies have shown a faster bone loss in patients with atherosclerosis than in patients without atherosclerosis.[30] However, conflicting results regarding these associations have been reported; several studies failed to show significant associations or even showed positive associations between BMD values and atherosclerotic parameters.[31,32] Thus, these associations seem quite dependent on the characteristics of the study population and measurements taken to evaluate atherosclerotic status. As yet, it is unclear whether these associations are based on the aging process or whether some specific biologic mechanisms may contribute to these associations.
In the present study, we observed potential associations between the presence of atherosclerotic plaque and low bone density. However, these associations were attenuated or even disappeared after adjusting for age; accordingly, it is conceivable that the aging process majorly contributes to the biological link underlying these inverse associations. However, interestingly, the association was stronger in calcified plaque and maintained statistical significance after adjusting for age. Calcified plaque severity also increased with decreased BMD T-score grade. This stronger and independent association between calcified plaque and BMD grade suggests that the pathology leading to calcified plaque formation also contributes to the link between atherosclerosis and osteoporosis, beyond the aging process.
The biological mechanisms connecting atherosclerosis and osteoporosis remain unclear as yet, but several possible explanations exist, including shared pathogenesis, such as aging, chronic inflammation, oxidative stress, and conventional risk factors that negatively affect both bone and vasculature.[7,33] Mediators between bone and vessels [5,34] and reduced blood supply to the bone [35] caused by atherosclerosis have also been proposed. Additionally, disturbed mineral metabolism, especially calcium and phosphorus balance, has been suggested to account for the association between lower BMD values and atherosclerosis, particularly with respect to vascular calcification.[33] Parathyroid hormone, vitamin D, fibroblast growth factor-23, and sex hormones are major hormones that regulate calcium and phosphorus metabolism in the human body.[36] Altered mineral metabolism promotes vascular calcification.[37,38] Additionally, disturbed mineral metabolism can result in higher parathyroid hormone levels, phosphonate levels, decreased vitamin D values, and lower BMD values. With the stronger and independent association between calcified plaque and lower BMD values, we cautiously suggest that mineral metabolism is crucial in the link between osteoporosis and atherosclerosis, in conjunction with aging. However, further studies are needed to elucidate the detailed mechanisms by which mineral metabolism may account for the inverse association between BMD and calcified atherosclerosis.
To the best of our knowledge, this study is the first to investigate the association between atherosclerosis and BMD values according to individual plaque characteristics as evaluated by CT. The strength of this study was the consideration of the severity of calcification and plaque characteristics in a large number of study participants, using CT scanning, which is a well-validated tool for characterizing plaque composition. However, there are some limitations to the present study. The BBC registry is a cohort of relatively healthy peri- and postmenopausal Asian women, which limits the generalizability of our results to other populations, such as men or individuals with different risk profiles. Furthermore, the menopausal status of the study subjects was not accessed in this study. Moreover, the BBC registry included the study population retrospectively in a consecutive manner and did not utilize an outcome-based design. Therefore, the number of participants with plaque was very small and underpowered to draw a firm conclusion.
In conclusion, there is an inverse association between low bone density and the presence of CAP, as assessed by CT. This association was stronger and age-independent for calcified plaque but was attenuated for non-calcified and mixed plaque after adjusting for age. Further investigations are required to confirm these character-specific associations between osteoporosis and atherosclerosis, and to explore the biological links between calcified plaques and low bone density.
Acknowledgments
The clinical trial is registered with ClinicalTrials.gov, using the identifier NCT03235622. Details can be found at https://clinicaltrials.gov/ct2/show/NCT03235622?cond=NCT03235622&draw=2&rank=1
Notes
Authors’ contributions
Conceptualization: KMK, YEY, BLY, and JS; Data curation: KMK, YEY, and BLY; Formal analysis: KMK and YEY; Methodology: KMK, YEY, BLY, and JS; Writing - original draft: KMK and YEY; Writing - review & editing: KMK, YEY, BLY, and JS; All authors read and approved the final manuscript.
Ethics approval and consent to participate
This study was conducted in accordance with the principles of the Declaration of Helsinki, and was approved by the Institutional Review Board.
Conflict of interest
No potential conflict of interest relevant to this article was reported.
Funding
This research was supported by a Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT & Future Planning (NRF-2014R1A1A3051310) to KMK, and a grant from the Seoul National University Bundang Hospital Research Fund (Grant No 13-2018-001) to YEY and KMK, and a research grant from Hanmi Pharm. Co, Ltd (Grant No 06-2018-299) to YEY. The funders had no role in the design and conduct of the study, the analysis and interpretation of the data, or the review or approval of the manuscript.