Prevalence and Risk Factors of T-Score Spine-Hip Discordance in Patients with Osteoporotic Vertebral Compression Fracture
Article information
Abstract
Background
T-score discordance between the spine and hip is commonly observed when dual energy X-ray absorptiometry (DXA) is used to diagnose osteoporosis. However, information is scarce regarding the prevalence and risk factors for this problem in Korea. This study evaluated the prevalence of major/minor discordance and associated risk factors in elderly Korean patients with osteoporotic vertebral compression fractures (OVCFs).
Methods
This study included 200 patients (37 men, 163 women) treated for thoracic or lumbar compression fractures between January 2015 and August 2021. DXA was performed to examine T-scores and determine the prevalence of discordance, defined as a difference between the T-score categories of the femur and spine in the same individual. The t-tests, χ2 tests, and regression analyses were used to assess the associated risk factors of T-score discordance among the subjects.
Results
T-score concordance, minor discordance, and major discordance were observed in 137 (68.5%), 59 (29.5%), and 4 (2%) patients with OVCFs, respectively. The spinal T-score was lower than the femoral T-score in all major discordance and 81.3% (48/59) of minor discordant cases. Overall, the only factor related to T-score discordance was the age at fracture (odds ratio, -0.01; P=0.014).
Conclusions
The results of this study showed that a significant number of subjects (31.5%) showed spine-hip discordance, even with a mean age in their 80s. More attention should be paid to the appropriate evaluation and management of elderly patients with OVCFs. Moreover, a longitudinal study is necessary to verify the clinical importance of T-score discordance in this population.
INTRODUCTION
Bone mineral density (BMD) assessed by dual energy X-ray absorptiometry (DXA) is used to diagnose osteoporosis, assess fracture risk, and monitor changes in BMD over time.[1,2] The International Society for Clinical Densitometry (ISCD) has recommended that BMD should be measured for the purpose of diagnosing osteoporosis at 2 preferred skeletal sites, the hip and lumbar spine.[3,4] ISCD also recommended osteoporosis would be diagnosed on the basis of the lowest T-score for BMD found at the spine, total hip, and femoral neck.[5] However, clinicians commonly conflict the discordance of T-score category at the 2 different skeletal sites (lumbar spine and hip), which can complicate the diagnosis of osteoporosis and therapeutic plan.[6,7]
Discordance in diagnosis of osteoporosis is defined as the presence of different categories of T-scores in 2 skeletal sites of an individual patient.[8,9] This phenomenon can be divided into 2 types. Minor discordance refers to a difference of at least 1 category and if the difference is more than one diagnostic class (osteoporosis at one site and normal at the other site), it is referred to as major discordance.[6,10,11]
According to previous literatures, the prevalence of major T-score discordance is between 2.7% and 4.3%, whereas minor discordance is between 35% and 41%.[12,13] Various studies have analyzed the prevalence and impact of T-score discordance on the management of osteoporosis. The offset was found to significantly affect fracture risk with a hazard ratio of 1.12, independent of the fracture risk assessment tool (FRAX) probability.[14] However, studies on the prevalence and factors of T-score discordance in Korea are lacking, especially in patients with osteoporotic vertebral compression fractures (OVCFs).
Thus, we aimed to determine the prevalence and risk factors of discordance between hip and spine BMD using DXA among patients with OVCFs.
METHODS
1. Included patients
We carried out a retrospective review of patients diagnosed with OVCFs under the official approval of the Institutional Review Board (IRB; IRB no. EUMC 2021-10-031). From January 2015 to August 2021, Between 2011 and 2020, patients aged >65 years who were admitted for surgery due to acute
The 48 hip fracture were eligible for this study we identified 296 patients who were treated with spine compression fracture. We excluded women who were treated with significant glucocorticoid or aromatase inhibitor exposure (>90 days) in whom management differs from the general population.
A fracture was defined as a case in which the anterior or median height of the vertebra was decreased by more than 20% compared to the posterior height.[15,16] When it was difficult to differentiate from old fracture, it was diagnosed after magnetic resonance imaging evaluation. The OVCFs were properly treated based on current treatment principles including conservative treatment and surgical treatment. For these patients, systemic disease and fractures were checked with the medical records, and after reviewing the radiology department, 7 patients who had pathologic vertebral fractures and 66 patients were without DXA were excluded from the list, and 200 patients were finalized (Fig. 1).
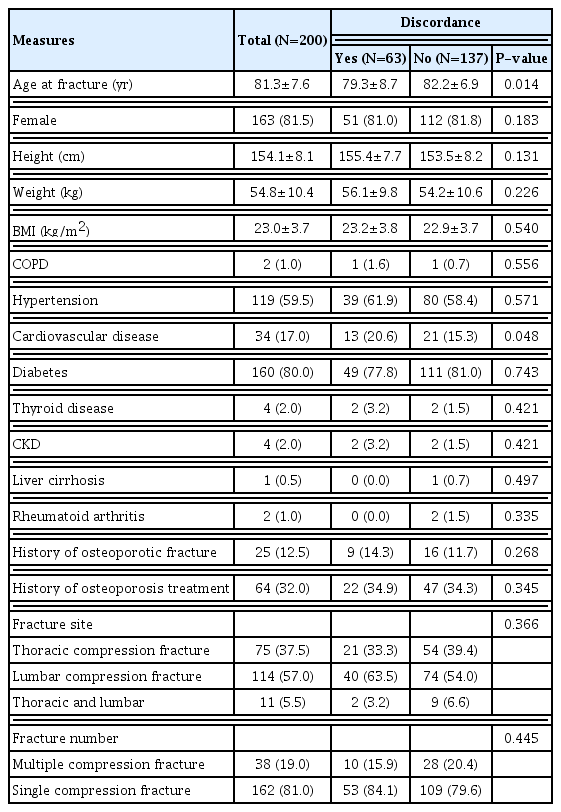
There were 75 Thoracic compression fractures (37.5%), 114 Lumbar compression fractures (57%), 11 were thoracic and lumbar compression fractures (5.5%). There were 162 single compression fractures (81%) and 38 multiple compression fractures (19%). Twenty-five patients (12.5%) had a history of previous osteoporotic fracture and 64 patients (32.0%) had been treated with osteoporosis treatment. Other demographic data are presented in Table 1.
2. Definition of T-score discordance
BMD of the lumbar spine and hip (total hip and femur neck) was measured using a Lunar Prodigy scanner (Lunar Prodigy; GE Medical Systems, Madison, WI, USA). Daily calibration and quality assurance testing were performed, and the BMD precision was lesser than 0.1%. We used the mean lumbar spine areal BMD value from at least 2 evaluable vertebrae from L1 to L4, and if there was a fracture, focal structural defect or a discrepancy of >1 standard deviation in T-score between adjacent vertebrae, the physicians excluded that vertebral level. The femoral neck and total hip T-scores were measured in the both (unfractured if injured) femur, and the lowest score at either site was used as the femoral T-score for the analysis. All densitometry was performed within 2 weeks after fracture occurrence. A T-score below −2.5 was considered osteoporosis; between −1 and −2.5, osteopenia; and more than −1, normal were diagnosed according to the World Health Organization (WHO) criteria. T-score discordance was defined as different WHO T-score categories at the 2 skeletal sites (femur and spine) of the same individual.[17] The patient was considered to have minor discordance when the difference was no greater than 1 WHO category and major discordance when 1 skeletal site was osteoporotic and the other was normal.[18,19]
3. Outcome variables
We evaluated the prevalence of T-score discordance in patients with OVCFs and also investigated demographic differences between the T-score concordance and T-score discordance groups. To determine associated risk factors for T-score discordance, we assessed medical conditions affecting osteoporosis were questioned including age of menopause, hypertension, angina or even myocardial infarction, rheumatoid arthritis, chronic obstructive pulmonary disease, diabetes, thyroid disease, renal failure, liver cirrhosis.[20] History of osteoporotic fracture and osteoporosis treatment were also investigated.
4. Statistical analysis
According to the normal distribution, Student’s t-tests or Mann-Whitney U test was used to compare continuous data, and the χ2 test or Fisher’s exact test was used to analyze categorical data. For all other tests, a 2-sided P-value of 0.05 was considered significant. To determine the risk factors of discordance, multivariable regression analysis was performed in variables with a P-value less than 0.1. Statistical analyses were conducted with STATA software (version 14.0; Stata Corp., College Station, TX, USA). The level of significance was set at P of less than 0.05.
RESULTS
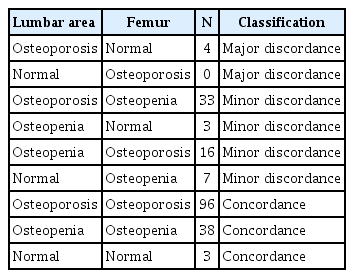
Based on the femoral neck, osteoporosis was found in 122 patients (61%), osteopenia in 67 patients (33.5%), and normality in 11 patients (5.5%). Also, osteoporosis was determined by the bone density of the lumbar vertebrae in 143 patients (71.5%), osteopenia in 45 patients (22.5%), and normality in 12 patients (6%). In all cases, T-score was inconsistent in 63 out of 200 cases was 31.5%. Among them, there was a major disagreement in 4 cases (2%), with all cases classified as having osteoporosis in the anteroposterior lumbar vertebrae but normal in the femur neck. In remaining 59 minor discordance cases, 48 patients (81.3%) had a spinal T-score that was lower than their femoral T-score (Table 2).
Sex, history of osteoporosis treatment and osteoporotic fracture, fracture location/number, weight, height, body mass index and several comorbidities did not differ between the concordance and discordance groups (Table 1). However, the age at fracture and cardiovascular disease did differ significantly between these groups. In the multivariable analysis, the age at fracture was an independent solitary risk factor for discordance (regression coefficient, −0.01; 95% confidence interval [CI], −0.002 to −0.018; P=0.014) but cardiovascular disease was not (odds ratio, 1.04; 95% CI, 0.47–2.31; P=0.402).
DISCUSSION
The reason why measurement of bone density by region is necessary is that, there is considerable inconsistency in bone density by region, so, the risk of fracture is considered to be different by region.[21] The spine is mainly composed of trabecular bone, so it has a fast metabolic rate and is sensitive to changes in the body environment, otherwise, femur neck BMD is associated with a higher gradient of risk for hip fracture than BMD measurements at other sites, with similar or better prediction of major fractures.[8] Thus, the lumbar spine and femur are preferred when measuring bone density.[22] However, the combination of these 2 skeletal regions could cause some problems for clinicians in decision making when there is a large discrepancy in the T-scores at these 2 regions in a given individual.[9,23]
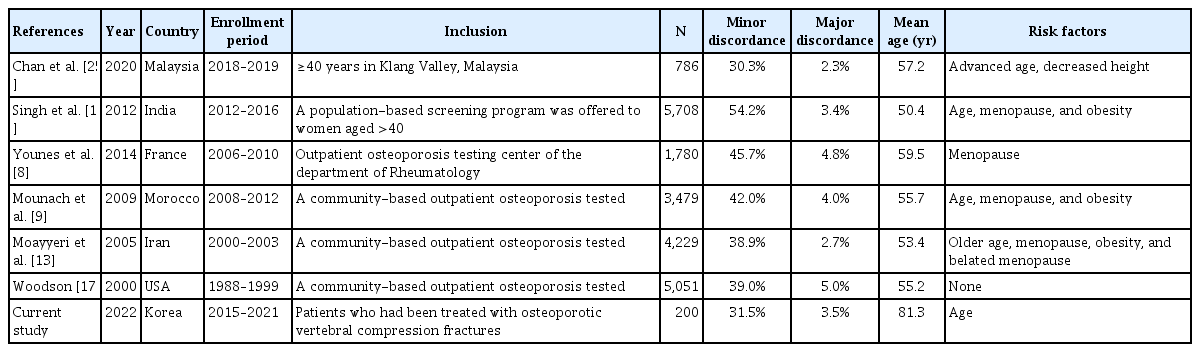
To the best of our knowledge, this is first study that evaluated the prevalence of spine-hip T-score discordance in Korean patients with OVCFs. A proportion of 31.5% in our patients showed T-score discordance between lumbar spine and hip, whereas only 3.3% (2/61) of the discordance cases were major discordance. These results are comparable to previous studies of postmenopausal women that found minor discordance in 30% to 50% of postmenopausal woman and major discordance in less than 5% of these. The results of our sample of patients are tabulated and compared with those of previous studies in Table 3.
Most subjects having discordance in our study (all major discordance and 81.3% of minor discordance) showed lower lumbar spine BMD compared to hip BMD. Reduced BMD at the lumbar spine tend to be more prevalent compared to that at the hip in 60 and 70 years of age. However, T-score of the spine tend to reverse that of the hip in the elderly over 80 years of age due to degenerative changes in the lumbar spine and calcification of the aorta.[14,24] Since the average age of this study was in their 80s, a different pattern of spine-hip discordance was expected but not. Clinicians need to be aware of the possibility of spine-hip discordance in the age group over 80 and carefully examine the risk group of OVCFs.
Discordance was found to be highest incidence in the elderly group especially in 60s and decreased from the 70s in general population. Chan et al. [25] reported discordance was about 32% and found highest in people in their 60s (47%). It is explained that discordance is that created by the different rates of bone loss, and the rapid bone loss due to menopause is most prominent in the 60s of post-menopausal osteoporosis.[25–27] In our study, the age at fracture was the only independent solitary risk factor for discordance with negative regression coefficient of −0.01. This negative correlation is line with the results of previous studies, because the average age of this study is in their 80s and the discordance is highest in their 60s.
As compared to hip fractures, vertebral fractures have often been underestimated in clinical practice. One study that compared the effectiveness of femoral neck and lumbar spine BMD for estimation of the risk of vertebral fractures using FRAX.[24] Because FRAX adopts only femoral neck BMD for calculating fracture risk, the risk of major osteoporotic fracture might be underestimated when the lumbar spine T-score is much lower than the hip. For example, if 2 individuals had identical femur neck T-score but different lumbar spine T-scores would generate the same fracture risk under FRAX. Thus, when confronted with highly discordant measurements (lumbar spine worse than femoral neck) in patients aged 7 to 80 years, clinicians should be alerted of the risk of OVCF and focused on lowering offset between the lumbar spine and femoral neck.[28]
The present study has some limitations. First, the design of our study was single center, retrospective and included number of patients were relatively small. Second, the cause of discordance can be classified into physiologic, pathophysiologic, and artifacts but we did not evaluate the possible causes for discordance in this study.
CONCLUSION
The spine–femur BMD T-score discordance was demonstrated in approximately 32% of Korean elderly patients with OVCFs even with their mean age of 80s. Considering the worldwide increase of the aging population, more attention should be paid to the appropriate evaluation and management of subjects with hip-spine BMD discordance. Also, a longitudinal study would be necessary to verify the clinical importance of T-score discordance in this group.
Notes
Ethics approval and consent to participate
This study was conducted according to the principles expressed in the Declaration of Helsinki and was approved by the Institutional Review Board (IRB no. EUMC 2021-10-031).
Conflict of interest
Byung-Ho Yoon has been the associate editor of the Journal of Bone Metabolism since 2015. No potential conflict of interest relevant to this article was reported.