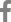|
 |
| jbm > Volume 26(3); 2019 > Article |
|
Abstract
Background
Treating patients with osteopetrosis is very challenging even in very skilled surgeons with many experiences. We present an account of 5 patients treated for hip fracture related problems occurring throughout their life due to this disease. Difficulties encountered during their treatment prompted us to present some general management principles.
Methods
From January 2003 to December 2016, 5 patients with osteopetrosis (9 hips; 3 men, 2 women), who underwent operative or conservative treatment were retrospectively reviewed. We evaluated their clinical features and rate of union, malunion and post-operative infection.
Results
Four of 5 patients (80%) suffered bilateral fracture, and 8 of 9 fractures (89%) are transverse and occurred at subtrochanteric area resulted from minor trauma. Among 9 hips, surgery was performed in seven hips. Nonunion were found in 3 hips (33%), malunion in 1 hip (11%) and oteomyelitis was developed in 2 hips (22%) at a median of 8.1 years.
Osteopetrosis is a rare hereditary bone disorder characterized by hard and brittle marble bone due to a defect in the function of osteoclasts.[1] This disease is generally divided into 3 types: (1) infantile malignant autosomal recessive; (2) intermediate autosomal osteopetrosis; and (3) benign autosomal dominant.[2] Increased bone density and frequent fractures are the clinical findings in the second group, and the third group which have normal life expectancy.[3]
The long bones are most frequently affected, fractures of the femoral neck and proximal (upper third) shaft being particularly common.[4,5] And these fractures are often result from minimal trauma even though the patients are very young.[6,7] Operative intervention needed in this area but physicians usually presents with unique technical challenges.[8,9,10] Difficulties during their treatment encountered include iatrogenic fracture during implant placement, overheating and breakage of drills and saws, increased risk for osteomyelitis or nonunion.[11]
There are only few studies about hip fracture in patients with osteopetrosis, and most of these are case reports or descriptions of treatment in surgery on mixed fractures. To our knowledge, there has been no case series of hip fracture in adult patients with osteopetrosis, and we could not find any investigations aid in hip fracture management of these patients.
We therefore reviewed a group of patients with osteopetrosis who underwent hip fracture surgery from multi-center to assess (1) clinical presentation (fracture pattern and bilaterality); (2) prognosis (radiographic and clinical union rate, infection rate, refracture rate). This case series propose possible operative treatment in patients with osteopetrosis and highlights the potential peri-operative pitfalls in this rare surgical population.
From January 2003 to December 2016, 12 patients with osteopetrosis data from 4 tertiary referral hospitals were retrospectively reviewed. Patients who had not hip fracture or had infantile autosomal recessive are all excluded because these patients usually treated conservatively and courses different clinical manifestations. Finally, 5 adult patients (9 hips; 3 men, 2 women), who underwent operative treatment were retrospectively reviewed. Patients were informed that their medical data could be used in a scientific study.
All internal fixations using dynamic hip screw or locking plate were performed in a standard basic technique. The patients were placed in a supine position on a fracture table. Open reduction using an image intensifier was performed in all patients. After discharge, patients were routinely followed up at 6 weeks, 3, 6, and 12 months post-operatively and annually thereafter. When a patient had not returned on regularly scheduled visits, the patients or their family was contacted by telephone.
We identified the configuration of fractures on conventional anteroposterior and lateral radiographs to describe their feature. Radiological union was considered to be obtained when 3 of the 4 cortices had a bridging callus in the anteroposterior and lateral views. Union in radiographs obtained at 6 weeks were done by 2 independent observers (JYL, BSK) who had not participated in the operations. Clinical union was considered to be obtained when patients had no pain during walking and palpation and radiographs showed no evidence of screw loosening or fracture displacement. Malunion was defined as an anteroposterior or mediolateral deviation of >5 from anatomic norms. Major local complications including wound infection and osteomyelitis were also evaluated.[12] Descriptive statistics were reported as median and range for continuous variables and as total number and percentage for discrete variables. The design and protocol of this study was approved by the Institutional Review Board for human research at each hospital.
The median age of the patients at the first time of hip fracture was 36 years (range, 30-43 years) and all patients were followed for a minimum of 4.5 years (median, 8.1 years; range, 4.5-15 years). All patients had a previous fracture history other than hip and 4 patients involved bilateral sites.
Among 9 hips, transverse pattern fracture occurred at subtrochanteric area in 8 hips and femur neck in 1 hip. Surgery was performed in 7 hips, and extramedullary plates (dynamic hip screw or locking plate) were used due to difficulty creating medullary canal (Table 1). The bone union rate was 66% (6 in 9 hips); Seven of 9 hips were operated on and four of them were fused, and 2 hips were healed with conservative treatment but one was accompanied by malunion. The osteomyelitis occurred in 2 hips and 1 case of osteomyelitis of the proximal third of the femur had been treated with several repeated debridements and finally with femoral head resection (Fig. 1). One patient had been successfully treated with a dynamic hip screw for subtrochanteric fracture, but refracture occurred after complete union of at the tip of plate (Fig. 2).
Osteopetrosis is a disease which results into universal failure of the bone remodeling process and the fractures most commonly involve long bones such as femur.[2,13] Hip fracture surgery in patients with osteopetrosis is very challenging, because the bones are very hard with loss of medullary canal by insufficient resorption leading to excessive accumulation of bone matrix.[2,14] Although most of these fractures can be treated conservatively in child but operative fixation and urgent surgical treatment is crucial for adult patients.[15] However, if orthopaedic surgeons facing patients with these perplexing disease, even skilled physicians are reluctant to do surgery, because we don't know their prognosis and treatment results including the risk of infection or nonunion. To the best of our knowledge, this study has the largest number of treated hip fractures in patients with osteopetrosis, and we noticed that 6 of 9 hips (66%) reported being union at final follow up.
Several reasons may explain the predominance of high nonunion rate after surgery in these patients. Blood supply are deteriorated so non-union of periarticular fractures occur commonly in osteopetrosis.[16,17] Surgery is technically difficult, because there is a high incidence of breakage of instruments and implants during the surgery due to the hardness of the bone.[10] In addition, it may not be possible to add supplementary autologous cancellous grafts in delayed or non-union because of absence of available cancellous bone.[18]
All cases of achieving bone union in the cohort showed bone union within a period compatible with general patients (range, 6-10 months after surgery). Recent studies have shown that adult type 1 osteopetrosis is not true osteopetrosis and his is due to the mutation of the LRP5 gene, which leads to an increase in bone mass, which is not known to be associated with osteoclast deficiency.[6,19,20,21] We believe that hip fractures in milder forms of osteopetrosis can be successfully treated with surgery similar to that of general patients.[11,22]
Most of our patients sustained trivial trauma and had a transverse fracture configuration compatible with radiographic features of atypical femoral fractures.[23] De Palma et al.[14] reported the histology of fracture callus in a patient with autosomal dominant osteopetrosis, that they found microfractures were frequently noted, but remodeling did not occur. Osteopetrotic fractures do heal with unorganised woven bone but remodeling does not occur.[14,21,24] In our case, peri-implant fracture occurred in one hip, stress concentration at the distal area of the plate may lead to a refracture (Fig. 2). Yoon and Park,[25] Chawla and Kwek [26] reported high incidence of peri-implant stress fractures (25%) and recommended the use of longer plates to span the whole bone would be recommended by passing through the most varus area of the femur which lead to preventing stress concentration.
Operative treatment of osteopetrotic fractures typically is reported as associated with many complications. Two (22%) of 9 hips in our cases develop osteomyelitis. Osteomyelitis is common in patients with osteopetrosis because of a reduced resistance to infection, attributed to the lack of marrow vascularity and impairment of white cell function. Bhargava et al.[27] recommended frequent change of drill bits and periodic cooling of the bone while drilling to prevent bone necrosis and infection. The most common complication of nonoperative treatment is coxa vara deformity and we also observed in 1 case among conservatively treated 2 hips. In one case, malunion was involved, but both conservatively treated hips had bone union, nonoperative treatment should be considered as an option.[26]
There were several limitations in our study. First, our study was retrospective and involved a small number of patients. This limitation was unavoidable as a result of the rarity of these patients. Second, we did not perform genetic testing so could not confirm the type of osteopetrosis. Third, many different treatment options were involved and the length of follow up was not uniform for all patients.
To help readers who faced with similar embarrassing problems, we presented our cases. Since clinical features of hip fracture in patients with osteopetrosis are similar to atypical femoral fractures, it might be helpful to apply the principles of surgical treatment of atypical femoral fractures. However, patients should be informed of the possibilities of several anticipated complications including intra-operative and post-operative course and risk of infection after surgery.
DECLARATIONS
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
1. Cadosch D, Gautschi OP, Brockamp T, et al. Osteopetrosis-a challenge for the orthopaedic surgeon. S Afr J Surg 2009;47:131-133.

4. Parry MC, Povey J, Blom AW, et al. Comparison of acetabular bone resection, offset, leg length and post operative function between hip resurfacing arthroplasty and total hip arthroplasty. J Arthroplasty 2015;30:1799-1803.


5. Chung HC, Park SH, Kim ES, et al. A case of cavernous sinus thrombophlebitis and meningitis as a complication in osteopetrosis. J Bone Metab 2014;21:227-232.

6. van Hove RP, de Jong T, Nolte PA. Autosomal dominant type I osteopetrosis is related with iatrogenic fractures in arthroplasty. Clin Orthop Surg 2014;6:484-488.



7. Amit S, Shehkar A, Vivek M, et al. Fixation of subtrochanteric fractures in two patients with osteopetrosis using a distal femoral locking compression plate of the contralateral side. Eur J Trauma Emerg Surg 2010;36:263-269.



8. Huang J, Pan J, Xu M, et al. Successful open reduction and internal fixation for displaced femoral fracture in a patient with osteopetrosis: Case report and lessons learned. Medicine (Baltimore) 2017;96:e7777.



9. Ganz R, Grappiolo G, Mast JW, et al. Technical particularities of joint preserving hip surgery in osteopetrosis. J Hip Preserv Surg 2017;4:269-275.




10. Dawar H, Mugalakhod V, Wani J, et al. Fracture management in osteopetrosis : An intriguing enigma a guide for surgeons. Acta Orthop Belg 2017;83:488-494.

11. Aslan A, Baykal YB, Uysal E, et al. Surgical treatment of osteopetrosis-related femoral fractures: two case reports and literature review. Case Rep Orthop 2014;2014:891963.




12. Pulido L, Parvizi J, Macgibeny M, et al. In hospital complications after total joint arthroplasty. J Arthroplasty 2008;23:139-145.


13. Landa J, Margolis N, Di Cesare P. Orthopaedic management of the patient with osteopetrosis. J Am Acad Orthop Surg 2007;15:654-662.


14. de Palma L, Tulli A, Maccauro G, et al. Fracture callus in osteopetrosis. Clin Orthop Relat Res 1994;85-89.

15. Krieg AH, Speth BM, Won HY, et al. Conservative management of bilateral femoral neck fractures in a child with autosomal dominant osteopetrosis. Arch Orthop Trauma Surg 2007;127:967-970.



16. Bénichou OD, Laredo JD, de Vernejoul MC. Type II autosomal dominant osteopetrosis (Albers-Schonberg disease): clinical and radiological manifestations in 42 patients. Bone 2000;26:87-93.


17. Waguespack SG, Hui SL, Dimeglio LA, et al. Autosomal dominant osteopetrosis: clinical severity and natural history of 94 subjects with a chloride channel 7 gene mutation. J Clin Endocrinol Metab 2007;92:771-778.



18. Whyte MP, McAlister WH, Novack DV, et al. Bisphosphonate-induced osteopetrosis: novel bone modeling defects, metaphyseal osteopenia, and osteosclerosis fractures after drug exposure ceases. J Bone Miner Res 2008;23:1698-1707.


19. Kilian O, Kriegsmann J, Hansen T, et al. A benign form of osteopetrosis. Case report. Unfallchirurg 2001;104:1014-1019.



20. Manzi G, Romanò D, Moneghini L, et al. Successful staged hip replacement in septic hip osteoarthritis in osteopetrosis: a case report. BMC Musculoskelet Disord 2012;13:50.




21. Wang C, Zhang H, He JW, et al. The virulence gene and clinical phenotypes of osteopetrosis in the Chinese population: six novel mutations of the CLCN7 gene in twelve osteopetrosis families. J Bone Miner Metab 2012;30:338-348.



22. Kumbaraci M, Karapinar L, Incesu M, et al. Treatment of bilateral simultaneous subtrochanteric femur fractures with proximal femoral nail antirotation (PFNA) in a patient with osteopetrosis: case report and review of the literature. J Orthop Sci 2013;18:486-489.


23. Shane E, Burr D, Abrahamsen B, et al. Atypical subtrochanteric and diaphyseal femoral fractures: second report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 2014;29:1-23.


24. Dong L, He W, Huo S, et al. The failure experience of complex total hip arthroplastyin osteopetrosis: case report and literature review. Int J Clin Exp Med 2015;8:14727-14731.


25. Yoon BH, Park SB. Insufficiency fracture occurring 3 years after union of an intertrochanteric hip fracture: A case report. JBJS Case Connect 2017;7:e1.


Fig. 1
(A) An anteroposterior view of the pelvis obtained at the time of injury shows a right transverse subtrochanteric fracture and osteosclerotic appearance of the osteopetrotic bone. The patient suffered a postoperative infection after surgery of left femoral neck fracture. (B) Radiographs at 4 years after injury shows a healed right subtrochanteric fracture with coxa vara. The chronic osteomyelitis of left hip finally treated with Girdlestone operation.

Fig. 2
(A) An anteroposterior view of the pelvis obtained at the time of injury shows a transverse subtrochanteric fracture in left hip. He had been treated with subtrochanteric fracture at the right hip (contralateral limb) 8 years ago. (B) Postoperative anteroposterior radiographs obtained 1.2 years after surgery shows refracture occurred at the tip of plate. (C) Refixation using long dynamic hip screw plate was performed and the radiograph showed complete union of the fractures at 12 months postoperatively.
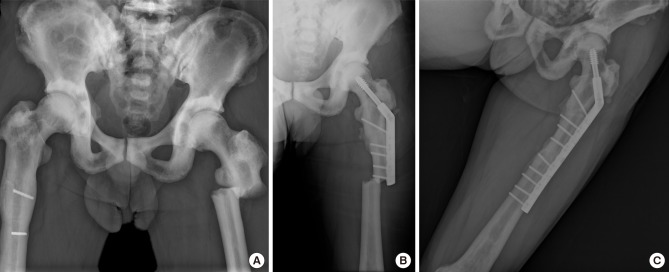
Table 1
Operative details of patients
a)Time from first fracture to contralateral side.
M, male; F, female; BMI, body mass index; F/U, follow-up; OR/IF c DHS, open reduction and fixation using dynamic hip screw; OR/IF c LCP, open reduction and internal fixation using locking compression plate; OR/IF c MS, open reduction and internal fixation using multiple cannulated screws.
- TOOLS




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print